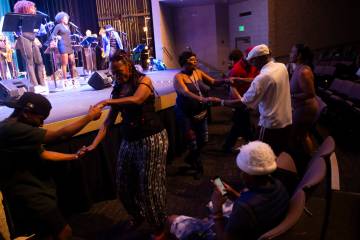Goaltender Logan Thompson shined in net as the Golden Knights defeated the Dallas Stars on Wednesday to take a 2-0 lead in their first-round playoff series.
Tropicana owner Bally’s Corp. filed for a commercial demolition permit this month with Clark County as preparations continue to build a ballpark for the Oakland Athletics.
Two Henderson parents have been arrested on suspicion on child abuse after police found an 11-year-old inside a large metal enclosure inside a residence.
University Medical Center defends the $115,200-a-year contract of an influential doctor, but the public hospital can’t document cases he has reviewed.
Bishop Gorman announced Wednesday that its baseball team was forfeiting games over paperwork related to the eligibility of a transfer student.
A ’70s theme for the evening celebration proved fitting, given that the library first opened in a tiny storefront in 1973.
The city’s mobsters roots run deep. Here are a list of mob-connected homes that has sold in recent years, including one formerly owned by Frank “Lefty” Rosenthal.
Tom Telesco begins his first draft in charge of the Raiders on Thursday. Turning the team around starts with getting better results with the team’s selections.
At 84, Smokey Robinson is still fit and a master of his performances.
Famous rock climber Alex Honnold joins Rep. Susie Lee in outdoor recreation panel, highlighting legislation that passed the House.
Nevada’s history is full of temblors. On average, about 10 earthquakes a day occur in the Silver State.
DeAjai Guaydacan was arrested Tuesday in Spanish Fork, Utah, and booked into the local county jail on suspicion of open murder pending extradition to Las Vegas.
The crane was being used in the $600 million Las Vegas Convention Center renovation project at the facility’s North Hall.
The Golden Knights and Dallas Stars are creating one of the best rivalries in the Western Conference after meeting in the playoffs for the third time in five years.
April is World Wish Month! It is a time when the world comes together to make dreams come true for children facing critical illnesses. As long as these brave kids need hope and strength, wish makers like you are essential to their fight. Speaking of wish-making, here’s an exciting opportunity: Walk For Wishes® 2024! Presented […]





After just over a year, former Raiders tight end Darren Waller and Aces guard Kelsey Plum have called it quits on their marriage.
The 100,000-square-foot center, replacing an aging office complex, will include restaurants, culinary kiosks and a covered alfresco dining lounge.
Terry Fator is using new architecture at The Strat Showroom to his advantage. That venue is part of the resort’s $125 million overhaul under owner Golden Gaming.
A motorcyclist was killed after a crash with a pickup truck in North Las Vegas.