UMC doctor’s dedication inspiring
When nurse Abby Hudema talks about why the University Medical Center pediatric intensive care unit staff follows infection control policies so closely — it was one of only five such units nationwide to earn the Consumer Reports’ top rating for preventing bloodstream infections in 2012 — she recalls a scene that at first blush doesn’t seem to have much to do with preventing bacteria from entering the bloodstream.
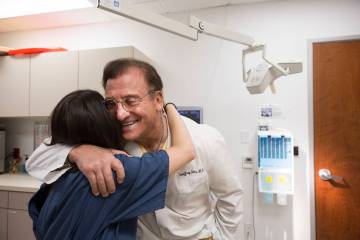
Dr. Meena Vohra, medical director of the pediatric ICU as well as chief of pediatrics at UMC’s Children’s Hospital of Nevada, walked out of a tiny patient’s room with dark circles under her eyes and a weary smile on her face, greeting the other doctors and nurses before leading morning rounds.
“You knew she was exhausted, she’d been at the bedside all night to keep the child alive,” said Hudema, the pediatric trauma program coordinator. “Yet she was upbeat on rounds, always asking questions about why this had or hadn’t been done.”
Hudema, whose department often first treats patients who end up in the pediatric ICU, believes it’s Vohra’s passionate commitment to patients’ welfare, including never cutting corners when it comes to hand washing and always wearing gloves, gown and mask when inserting a central-line catheter, that has created an attention-to-detail medical staff, one so engaged that the UMC unit experienced zero central-line associated bloodstream infections over a yearlong period.
Not even Minnesota’s Mayo Clinic or St. Jude Children’s Research Hospital in Memphis, Tenn., did that.
“Dr. Vohra never asks someone to do something she doesn’t do,” said Hudema, a 22-year nursing veteran. “She leads by example. Her staff then shows the same commitment.”
Studies show 250,000 central-line infections occur each year, resulting in 31,000 deaths and $9 billion in increased costs.
Too often, researchers find, there isn’t careful disinfection of the catheter insert site, dressings aren’t regularly changed, catheters are kept in too long.
“The way I look at it,” Vohra said, “if the leader follows the rules, everybody does. You have a domino effect.”
Now 56, Vohra began at UMC in 1991, then the only physician there trained in pediatric critical care. Often, she’d be called in at night. Because her husband, cardiologist Dr. Sanjay Vohra, frequently was on call as well, she’d find herself taking their then young daughter, Anita, to work with her.
“We’ve come a long way since then,” said Vohra, who’s hired four pediatric critical-care specialists over the years.
Still, she works a 24-hour shift every five days. Dr. Jay Fisher, UMC’s head of pediatric emergency, says it’s unusual to find someone with her experience remaining on the front lines of pediatric critical care.
Burnout is common. Seeing children die and giving grief-stricken families news they never want to hear takes its toll.
“It’s a little atypical to see an intensive care physician at her age,” Fisher said. “She’s extremely fastidious, very careful, and expects that from everyone else.”
Often, Hudema said, you find Vohra teaching medical staff.
“That’s something I’ve seen fall by the wayside in my career, doctors really teaching,” Hudema said.
Vohra admits to being “very strict,” but is careful not to upbraid staffers in front of others.
“I’ll take them aside and we get things right,” she said.
Born and raised in India — she did graduate medical studies in Detroit — Vohra’s upbeat disposition makes it easier for her to deal with life and death.
When recalling that her husband began courting her by asking to play mixed doubles pingpong, she giggles like the teenager her youngest daughter, Sonia, is.
She always sees the glass as half-full. No, her dream of a free-standing pediatric hospital at UMC hasn’t come true, but spread out within UMC today is the only Level II pediatric trauma center in the state, the only pediatric emergency room in Las Vegas with board certified, fellowship-trained physicians on duty 24 hours a day, the state’s only pediatric burn care and transplant service, and Nevada’s only dedicated pediatric sedation unit.
“I don’t have time for dejection,” she said, laughing. “Too much to accomplish.”
Child advocates nationwide argue stand-alone children’s hospitals are needed because fragmentation of services in communities is not only inefficient, but difficult and sometimes impossible to navigate for frantic parents of ill children.
Although the Children’s Hospital Association lists more than 40 pediatric free-standing hospitals not affiliated with hospital systems, it doesn’t track the number of children’s hospitals affiliated with hospital systems that are in stand-alone centers. Spokeswoman Gillian Ray said, however, it is “definitely a model that is working.”
Vohra said she’s seen it work throughout the country.
“I’m working on getting funding for a new UMC pediatric hospital myself,” Vohra said. “We deserve the best for Nevada’s children.”
Contact reporter Paul Harasim at pharasim@
reviewjournal.com or 702-387-2908.