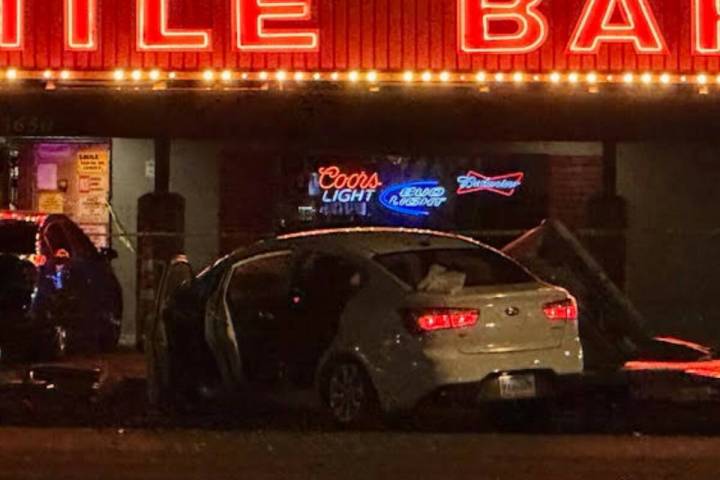Two pedestrians were killed and at least three were injured when a car crashed into a bus stop in the east valley.
Thirty-two more people have died in crashes on Clark County roadways this year compared with the same time in 2023, Nevada officials announced.
A Family Court judge ordered attorney Dylan Houston to turn in his guns as part of a temporary custody agreement involving the man’s young children.
About 30 robberies/attacks on letter carriers have occurred in the valley over the past three years, a National Letter Carriers Union spokesman said.
One casino has been a downtown Las Vegas staple for years. Another is set for a rebranding. Both reported million-dollar jackpots.
A man who told police he had shot at a truck carrying his stolen motorcycle outside his northeast valley apartment is facing a murder charge.
Bishop Gorman’s baseball team played its first game in Las Vegas since coach Chris Sheff was suspended and an investigation into the program began.
Grammy-winning musician Gwen Stefani took the stage to the roar of 400 partiers at Ole Red Las Vegas on the Strip.
Hilton has acquired a controlling interest of the operators of this hotel, but the deal excluded the Vegas location.
The Raiders had a surprising turnaround on defense last season, but they could still look to add on that side of the ball during this month’s NFL draft.
Clark County Republican Party Chairman Jesse Law was arrested on suspicion of domestic battery, but court records show the district attorney’s office has decided not to pursue the case.
Clark County officials “willfully” destroyed evidence related to a Red Rock housing development, a district court judge ruled.
Secretary of State Cisco Aguilar’s office released its first quarterly report of investigations into election fraud claims.
“I Am: Celine Dion” is due to begin streaming June 25 on Prime Video.
After announcing a promotion tied to an alternative team name, the Aviators saw record merchandise sales and pulled some of the items off their online store to sell at Saturday’s game.
Home Means Nevada—those are three words that every Nevadan knows. Aside from being the title of our state anthem, these words are plastered on bumper stickers, t-shirts and souvenirs across the Silver State. Nevada is renowned for its stunning natural landscapes and bustling entertainment scene and it continues to attract new residents drawn by its […]
The company that developed Omega Mart at Area 15 is cutting dozens of jobs at the off-Strip attraction.
The twin brothers accused in a firework attack on a Henderson LDS church have been linked to similar attacks on the church, police say.
The Vegas Golden Knights announced on Friday that the team will once again help local residents by giving away free gas.
Among the dishes: vegetarian bolognese, braised short rib with polenta and a pizza with three cured Italian meats.