10 things to know about dangerous Candida auris fungus
Candida auris, a potentially lethal fungus, has triggered the largest outbreaks in the country at Southern Nevada hospitals and long-term care facilities.
C. auris, as it’s often called, has spread at an “alarming rate” in the U.S., according to the Centers for Disease Control and Prevention. Southern Nevada last year reported the most invasive infections from the new pathogen, according to the Centers for Disease Control and Prevention.
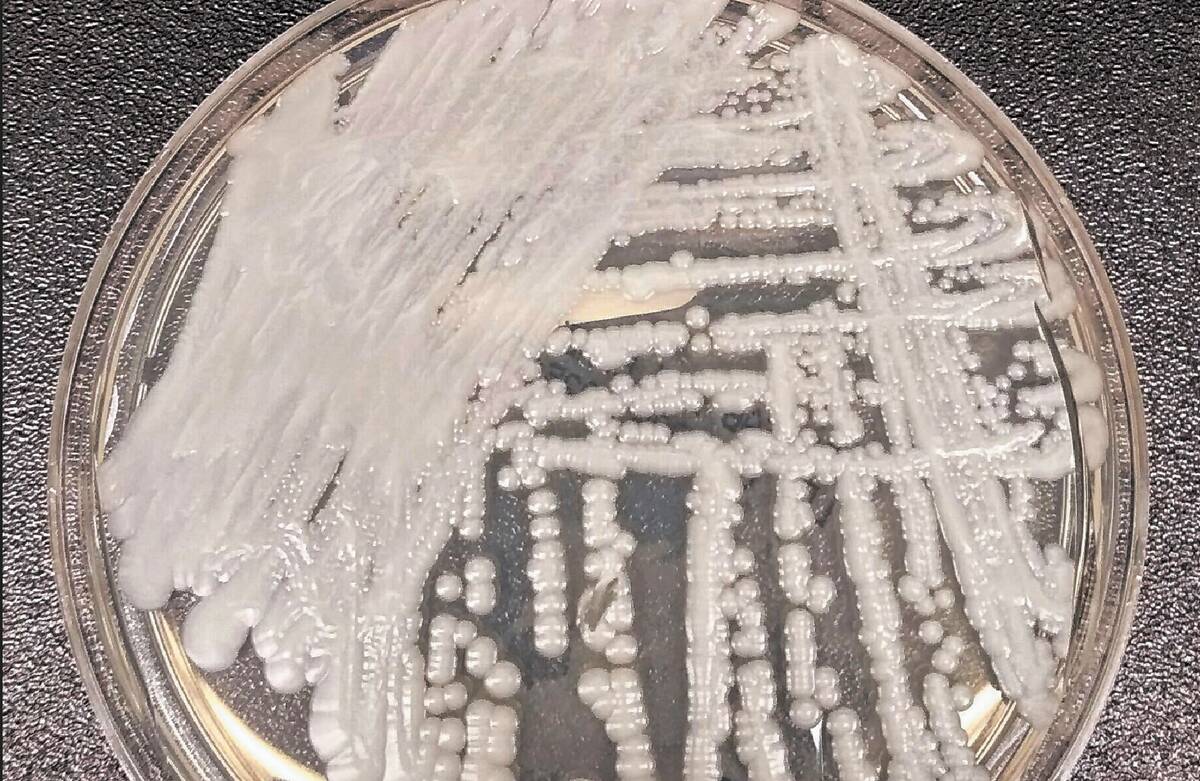
What is Candida auris?
Candida auris is a strain of yeast in the same family that causes thrush, a white rash in the mouth and throat, and vaginal yeast infections. C. auris was first identified in Japan in 2009 and in the U.S. in 2016. Cases were first detected in Southern Nevada in August of 2021.
How do people catch it?
C. auris can spread from person-to-person and also from contaminated surfaces or equipment. Most cases in the U.S. are spread within, and among, health care settings.
What are the symptoms?
The most common symptoms of an invasive infection of C.auris — such as one of the bloodstream, brain or heart — are fever and chills that don’t improve after antibiotic treatment for a suspected bacterial infection.
This fungus is sneaky. A person may have the fungus somewhere on the body without any signs or symptoms or making them sick, which is called colonization. A person who is colonized, despite not having symptoms, can still spread the fungus to other people.
Where on the body does it colonize?
CDC epidemiologist Dr. Meghan Lyman said C. auris most often colonizes the skin.
“It can also live in other body sites without causing infection, like the nose, urinary tract, or respiratory tract,” Lyman said in an email.
What does Candida auris look like on the skin?
In a colonized individual, it’s invisible to the eye. “There are lots of microbes, including bacteria and fungi, that live on the skin that cannot be seen visually,” Lyman said.
C. auris can also cause skin or wound infections. “The signs and symptoms would be similar to infections caused by bacteria, such as redness, swelling, and draining.”
How is C. auris diagnosed?
Diagnosing C. auris requires specialized lab tests. A colonization screening typically involves a swab test in the armpit and groin. As part of diagnosis and treatment of infections, cultures may be taken from other parts of the body, Lyman said.
Who is most at risk for an infection?
Healthy people usually don’t get C. auris infections. Patients who have been hospitalized for a long time, have a central venous catheter, or other lines or tubes entering their body, or have previously received antibiotics or antifungal medications, appear to be at highest risk.
“C. auris, like other germs on the skin, can cause invasive infections by entering breaks in the skin or mucosal barriers, such as stomach lining, the mouth/throat, and intestines, especially through indwelling medical devices, like central lines,” Lyman said.
More than one in three people who develop an invasive infection die, according to the CDC. Many have other serious medical conditions.
What is the treatment for C. auris?
Three types of antifungal medicines are commonly used to treat C. auris. A growing concern is that some C. auris infections are resistant to all three types of antifungals.
Does Candida auris go away in a colonized person?
“Patients with C. auris are often colonized for very long periods of time, even years, especially in those who remain in healthcare settings, but also in patients who have been discharged,” Lyman said. “However, there is still a lot to learn about the patterns of colonization and the possibility of clearing C. auris from the body.”
What is being done about C. auris?
Federal and state public health agencies are investigating the spread of C. auris and have stepped up screening for it in medical settings. They have recommended special cleaning protocols and other measures to prevent spread. Nevada’s congressional delegation has called for more federal resources to fight the fungus.
Contact Mary Hynes at mhynes@reviewjournal.com or 702-383-0336. Follow @MaryHynes1 on Twitter.