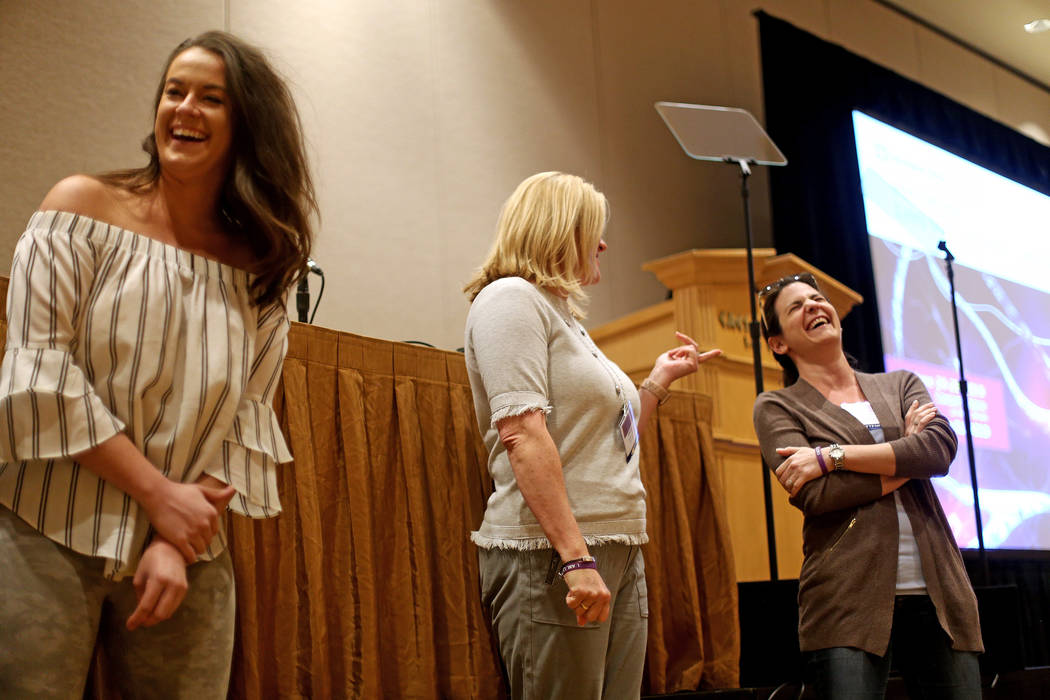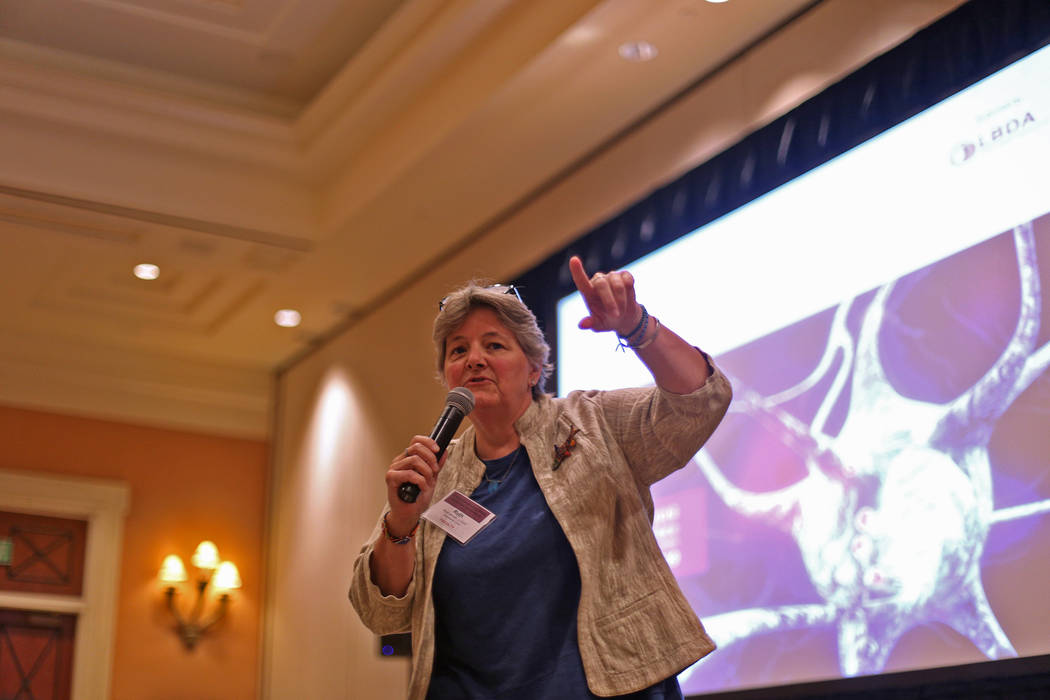Caregivers learn new tactics at Lewy body dementia conference
Five people stand in front of the room with an unusual assignment: Tell a story by building on whatever the person before them says.
The result isn’t completely smooth — the story begins with a dog at the hospital and ends with what seems to be a commentary about veterinary fees — but it does illustrate principles of the art of improvisation that might be useful the next time participants interact with a loved one or patient who has Lewy body dementia.
The improv exercise was presented during last week’s International Lewy Body Dementia Conference at Caesars Palace, hosted by the Cleveland Clinic Lou Ruvo Center for Brain Health. The conference offered caregivers, families, researchers and medical professionals the latest information about the degenerative brain disease in which proteins called Lewy bodies damage neurons, creating a raft of behavioral, cognitive and movement problems, including hallucinations.
Lewy body dementia, or LBD, is one of the most common causes of dementia in elderly patients, according to the clinic, and as many as 1.4 million people in the United States are estimated to have it.
Ruth Almén, clinical social work manager at the Ruvo center, said the improvisation curriculum was developed by Second City, the Chicago-based improv troupe, and Caring Across Generations, a caregiver advocacy group, in collaboration with the Cleveland Clinic and Ruvo Center.
“Their sense was that they could use basic improvisational principles … including the values of that process, to help caregivers,” she said.
For example, improvisation “requires really good listening. If you say something, my job is to take part of what you said and say something else,” Almén said.
In the tell-a-story exercise, participants couldn’t plan what to say because they didn’t know what the person immediately before them would say. But, Almén said, even with the inability to plan ahead that caring for someone with LBD brings, caregivers can try to be in the moment and “you can still get there.”
Listening closely and then building upon what someone else says also can promote communication with a loved one who has dementia. Say, for example, that a loved one insists that the animals he sees are real. Rather than trying to convince him that the animals are hallucinations — one common symptom of LBD — a caregiver might instead ask, “Didn’t you grow up on a farm?” to promote conversation where before there was frustration.
Almén said that after a session of classes last fall, caregivers reported that while their loved ones’ symptoms had worsened over a period of several months, the frustration and stress they felt either had been reduced or at least had not worsened.
The use of improvisational techniques can offer caregivers the benefit of spending more time with loved ones, Almén said. “I think what most caregivers want is time with their loved ones. They’re going to feel more comfortable and competent, and we can find ways to have those conversations and be together and enjoy more time.”
Las Vegan Mitzie Hiegel, whose husband, Larry McAlister, was diagnosed in 2016 with mild cognitive impairment consistent with Alzheimer’s or Lewy body disease, took the improv program last fall at the Ruvo center. She called it “very helpful. It was probably my first experience in being in the present, being in the moment.”
The couple learned about the LBD conference through a support group at the center that Hiegel attends, and found the daylong series of caregiver-oriented programs useful. Some of those presentations involved medical management issues, while others featured speakers sharing their own or loved ones’ experiences.
Robert Bowles of Georgia said he was diagnosed with LBD disease in 2012, at age 64, but that the diagnosis came only after a frustrating journey to eight doctors over 18 months. Bowles, a retired pharmacist and pharmacy owner, now considers it his mission to promote awareness of LBD.
Living with LBD means “not letting the condition define me,” he said. “We have to focus on living our lives.”
Not every day is a good one, but the goal is to “take advantage of the good days and use those good days to do something worthwhile.”
Katie Boer, a former Las Vegas TV journalist, moved to Seattle in August 2017 to care for her mother, who was diagnosed with LBD in late 2016. Although her mother was in an assisted living center and Boer talked with her several times a day, “it just got to the point where I couldn’t manage,” she said.
“I was doing 15 phone calls a day and (receiving) calls from my mother,” said Boer, who said her mother would say that she was “either being assaulted or attacked, or she’d just call me (with) hysteria, crying, giggling, and I’m trying to calm her...
“It just got to the point where it was really hard. I was living in Henderson at the time, and I’d go to sleep every single night in tears. I was so helpless,” Boer said. “I needed to be there. I needed to be present.”
Boer said that, in addition to hearing practical information about LBD, she found it comforting to hear others’ stories and meet patients and caregivers who live with it.
“I was sitting next to a guy who’s 71, who was diagnosed when he was 64, and he’s functioning so much better than my mom,” Boer said. “It’s not a club you want to be in, but there also is an incredible sense of, like, I don’t want to experience what they’re going through, but there is a sense of peace knowing you’re not alone.”
Contact John Przybys at jprzybys@reviewjournal.com or 702-383-0280. Follow @JJPrzybys on Twitter.
Las Vegas center has first clinical trial in offing
In a few months, the Cleveland Clinic Lou Ruvo Center for Brain Health is to begin its first clinical trial of a medication that someday might be used to treat Lewy body dementia (LBD).
LBD occurs when proteins in the brain attack neurons, causing symptoms that can include dementia, motor deficiencies and cognition problems. While it's similar to Alzheimer's disease and Parkinson's disease, it's not quite the same as either.
According to Dr. Aaron Ritter, director of the clinical trial program at the Ruvo center, Alzheimer's disease primarily presents with cognitive symptoms, while Parkinson's disease primarily presents with "motor symptoms, or all movement."
LBD can affect both cognition and movement, Ritter said, and with "new technologies like amyloid scans, we can make diagnoses a lot better."
However, misdiagnosis of LBD has been a hurdle to conducting clinical trials of potential LBD treatments. Attendees of last week's International Lewy Body Dementia Conference learned that a lack of qualified participants has prevented a few proposed studies from going forward.
"Getting enough people to participate in clinical trials is a challenge," Ritter said.However, "we are finally bringing some clinical trials here (for) Lewy body disease. We have observational studies, which are studies that are helping us to better understand … the disease, and also, for the first time, we're going to be having a treatment trial for Lewy body disease."
The trial is scheduled to start later this summer, Ritter said. "We're still going through the regulatory and legal process. But it's really exciting, because there have been very few symptomatic therapies for Lewy body disease tested in formal ways."
For more information about clinical trials at the Ruvo center, call 855-568-7886, email healthybrains@ccf.org, or https://tinyurl.com/y2ldtb58