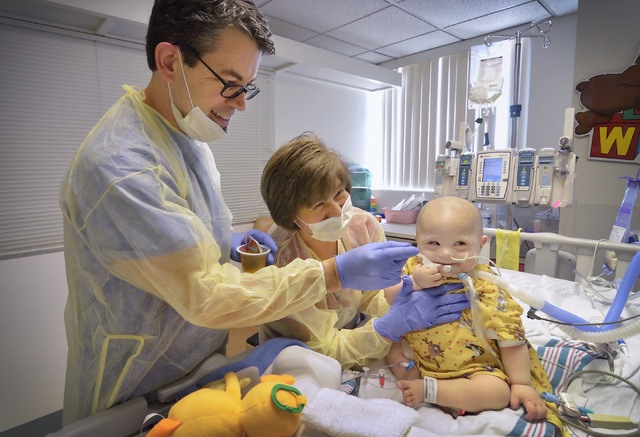
Speech pathologist shows injured and ill youngsters he cares
In a bleached and bleak hospital room, a baby wails.
Four-month-old Aprillyon Harper is dotted with tiny tumors. On his cheeks, beneath his chin, on his neck, in his brain. His mother paces the room as rain raps on the window, talking to child developmental specialists and high-risk pediatric social workers as her son’s little body writhes and cries.
He has just undergone chemotherapy, and now he is having trouble swallowing.
Beyond the room’s sealed door, Dale Whitman suits up. The pediatric speech pathologist covers his body in a gown, gloves and a mask. As he enters, the baby continues to shriek. All little Aprillyon can see is Whitman’s eyes, brightly blinking beneath his black frames.
“Hi there,” Whitman says softly.
Aprillyon stares, curious, then cries again.
Whitman kneels down, his glasses now at Aprillyon’s eye level.
“What’s your favorite food?” he whispers, knowing the baby boy cannot respond. “Rice? No. How about fruits? No?”
The boy’s mother, Rashonda Harper, 31, gives Whitman an odd look. The boy is sitting up now, unsure of what’s going on. Whitman keeps asking.
“Maybe applesauce? Pears?”
Aprillyon’s eyebrows curl up, perplexed, and his mother laughs at his puzzled reaction. He is still, but soon he cries again.
Whitman tugs his mask down and smiles. He lifts the boy up and onto his shoulder, and the tears cease.
The room is silent for the first time in the afternoon.
“Boy, you’ve got that magic touch,” says Aprillyon’s mother, Rashonda. “He likes you. He does not let anyone touch him without crying.”
Whitman laughs off Harper’s compliments as he holds her quiet baby in his arms.
“Maybe he thinks Dale is an overgrown kid,” says Jill Buckley, a social worker with Health Plan of Nevada who is sitting in the room.
Whitman, 42, has worked at University Medical Center for 12 years. Through playful exercises and encouragement, he teaches premature babies to suck and feed and coaches children with traumatic injuries and illnesses — children like Aprillyon — on how to swallow and eat again.
But not without a little fun.
“I’m kind of like the Nutty Professor,” he says.
■ ■ ■
In a sea of white coats, Whitman stands out.
His dark scrubs and red messenger bag are a familiar sight at UMC.
He is tall, and hovers above the rest as he travels from the neonatal intensive care unit to the pediatric intensive care unit and back to the pediatrics ward.
He is the kind of man who says “Hi” to everyone in the halls — doctors, nurses, supervisors, janitors. Every so often he reaches into his bag, offering a Starburst candy.
As Whitman walks, he talks about his wife, Maria, who works in the same field at St. Rose Dominican Hospital, de Lima campus. He mentions their three children, and how raising them helped make him better at his job.
But he is interrupted. A premature baby bundled in blankets and a beanie is wheeled past. Whitman stops to stare.
“Awww,” he says, watching the cart as it is wheeled into a back ward. “They’re always so cute, you know?”
Speech pathologists typically work at schools or hospitals, Whitman says.
Although his personality suggests he would have thrived in schools, his happy-go-lucky attitude is a welcome juxtaposition at UMC, where grim medical emergencies dominate everyday life.
The hospital is home to Nevada’s only burn care center and has the state’s only Level I trauma center.
“He’s always in a good mood and a very calming presence to the kids,” says Kimberly Grettum, a child care specialist in the burn unit who has worked with Whitman before.
“He’s quiet when he needs to be, and he meets the kids where they’re at. He doesn’t push them, but more like inspires them to get better and get them through their situation.”
In the pediatrics ward, Whitman goes to a small room where 4-month-old Dennis is lying on a bed. His mother, Lontesha Harrison, 24, is standing to the side, concerned. Her baby has been vomiting violently after meals, and she wants to make sure he is OK.
Whitman approaches the boy. He softly introduces himself and sits the baby up.
Dennis seems alert, a good sign.
Whitman holds up his finger, watching as Dennis’ eyes follow its movements.
He is attentive, and Whitman reminds everyone in the room that the boy is listening. He is small but he is smart.
Whitman traces the tip of his finger on Dennis’ stomach, pointing out that the organ is on his left side. He should eat slower and be burped on his mom’s right shoulder, so his left side is exposed and elongated.
Other than that, Dennis is just a fast eater, Whitman says.
“He’s my second, but you cannot get too much practice,” Harrison says.
As Whitman walks out, he explains how important the mouth is. It’s often taken for granted, but it’s how you speak, how you eat. And for new mothers, feeding is an infant’s first means of communication.
“It influences every developmental milestone on this planet,” Whitman explains.
If children can’t eat, parents can quickly feel like failures, he says, especially with those too young to speak.
“I like to give the parents jobs,” Whitman says, so they can take coaching skills home with them. “If this is Ground Zero, we need to somehow train the parents and give them the tools they need.”
Whitman says his strongest skill is that he cares.
“I don’t think you can fake that,” he says. “I don’t think you can go into a patient’s room and get the kind of reaction you need if you don’t care.”
■ ■ ■
Whitman works alone as UMC’s only pediatric speech pathologist.
He isn’t quick to take credit, but his role is one parents and young patients appreciate. His therapy is a crucial part of their pathway to recovery.
“Sometimes kids get stuck here for a long time,” Whitman says.
Several children lie on thin hospital beds, all hooked up. Wires dangle from their wrists and chests. Metal and plastic surround and encase them and monitors beep.
The television plays cartoons in the background, but there is no conversation until Whitman breaks the silence. He introduces himself and begins the assessment process.
“Can you sit up?” he asks. “Can you move your tongue back and forth?”
Whitman puts a Cheerio on the tip of his own tongue so it’s easier to track its movement.
“Watch me do this,” he says.
He opens his mouth, shifting his tongue from left to right, over and over. Again, the parents stare — confused yet entertained. And the children laugh. It’s routine.
“I don’t really care if they eat all their food,” Whitman says. “I’m going to get the right consistency of food for them, and I’m going to do it in a fun way.”
He reflects on the case of a 2-year-old internally decapitated and paralyzed from a horrific car accident. He was thrown from the car, Whitman says. He survived, but his neck snapped.
Because of his condition, Whitman was careful. Food is supposed to be comforting, but comfort can be worlds away in an environment such as the pediatric intensive care unit.
So he started with ice.
For two weeks, the speech pathologist brought in a SpongeBob ice maker, churning and grinding the ice as the little boy watched.
The 2-year-old couldn’t move, but he stared as Whitman repeated the process each day, becoming more and more comfortable.
“It has to be designed around play,” he said. “They’re the sickest of the sickest, the littlest of the littlest. I try to show them it’s not scary.”
One day, Whitman lifted the boy’s limp, immobile hand and touched it to the cold ice. Before he could let go, the boy flinched.
“I told the doctor,” Whitman said, who determined the patient’s paralysis was slowly fading in recovery.
“That kid is writing now.”