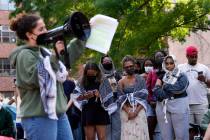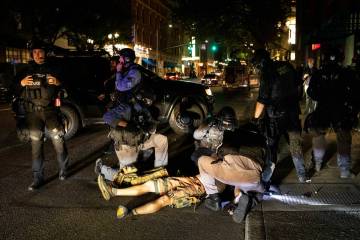The Oakland Athletics plan to build a ballpark on the site of the Tropicana, but Bally’s says where the stadium will sit on that site is still being determined.
Management of the Strip resort told the County Board of Commissioners the request relates to the construction timeline for the Oakland Athletics’ ballpark plan.
The Raiders are escaping the summer heat of Las Vegas for the coastal climate of Costa Mesa after coming to terms on a one-year agreement to hold training camp there.
Las Vegas police released recordings of the 911 calls related to a man who police allege later ate parts of a man’s face.
Red Rock Resorts says it will first focus on developing a California casino and then look at the second phase of its new resort in the southwest Las Vegas Valley.
Social media platforms have enabled critics to see just how twisted many of the woke pro-Hamas protesters are.
A controversial proposal for a Church of Latter-day Saints temple near Lone Mountain still has a ways to go in its quest for approval, city officials said.
Noted as the first tribal enterprise to manage a commercial casino in Nevada, the Mohegan group will turn over management to Virgin Hotels Las Vegas.
Former President Donald Trump called several potential vice presidential candidates onstage with him at a Republican National Committee fundraiser at Mar-a-Lago.
Clark County commissioners voted to award nine applicants a total of $66.25 million from a county housing fund.
Clark County received just one sidewalk vending license application during the first six days the ordinance was in effect.
The Golden Knights should do what’s best for the organization when it comes to pending free agent Jonathan Marchessault. That means re-signing him.
The Aces continue to make waves off the court this offseason, as their best player landed a major endorsement deal Tuesday.
The hotel-casino on the north Las Vegas Strip says the new promotion is meant to make the property more accessible.
The shooting occurred in the 1600 block of East St. Louis Avenue, east of Maryland Parkway in the early hours Tuesday, according to a Metropolitan Police Department news release.
Generosity: Any act of kindness or support given without expectation of exchange or return from the recipient(s). The game’s biggest stars remain active one month into the NFL offseason. They may not be running drills on the field, but they practice something more important: generosity. Hall of Fame quarterback Troy Aikman and 2022 NFL Man […]





The Sphere is taking a break from jam bands with a hockey-style shift change. The venue is hosting its first made-for-TV event in June, as the NHL draft plays to Las Vegas for the first time.
A CCSD substitute teacher punched a student at Valley High School in Las Vegas after the student called him a racial slur, according to an arrest report.
Commercial real estate experts weighed in on how much the property co-owned by Donald Trump and Phil Ruffin might sell for if it were put on the market.
The restaurant is owned by a big-name Vegas hospitality company with several other outlets in its portfolio.