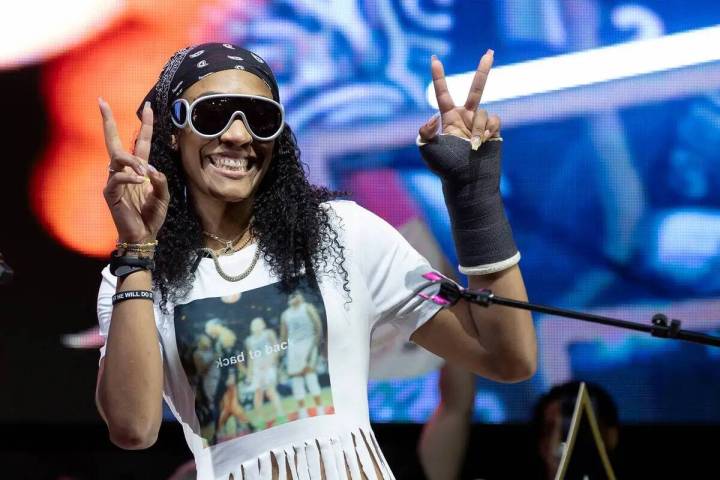Clark County School District police have arrested a man connected to a student-teacher fight at Valley High School on Thursday.
The Raiders drafted what could be a generational tight end in Georgia’s Brock Bowers, but they had other needs they should have addressed in the first round.
The Clark County School District is looking to make it easier to hire retired employees to fill “critical” vacant teaching, other jobs.
President Joe Biden will welcome the Las Vegas Aces to the White House on May 9 to celebrate their championship season, according to the White House.
The Las Vegas family attraction, which is aimed at kids ages 5 to 12, features 15,000 square feet of interactive dinosaur exhibits.
It would be hard to produce a less likely superstar than the singing impressionist Danny Gans, whose death on May 1, 2009, left a hole in this city that’s yet to be filled.
Matt McMullen has been at it for decades. His most realistic creation yet is a supermodel-esque woman with blonde-brown hair who speaks with a mild Scottish accent.
The wait is over. Here is who the Raiders picked in the first round of the 2024 NFL draft, and it came as a shock to many observers.
The 6:25 p.m. incident occurred in an apartment complex near West Tropicana Avenue and South Jones Boulevard.
Detergent and deodorant, toothpaste, the entire shampoo aisle. “It’s all locked up,” Corey Potter sighed.
Sick New World, Holo Holo and the Water Lantern Festival lead this week’s Las Vegas entertainment lineup.
Most Regional Flood Control District gauges showed from .04 to .12 of an inch for most parts of the valley. The temperature dropped 10 degrees in less than two hours before noon.
In-N-Out’s “secret menu” includes items ranging from pimped-out cheeseburgers to something called a whole grilled onion.
The crash occurred near Galleria Drive and Dave Wood Circle, north of East Lake Mead Parkway.
Generosity: Any act of kindness or support given without expectation of exchange or return from the recipient(s). The game’s biggest stars remain active one month into the NFL offseason. They may not be running drills on the field, but they practice something more important: generosity. Hall of Fame quarterback Troy Aikman and 2022 NFL Man […]





Tropicana owner Bally’s Corp. filed for a commercial demolition permit with Clark County as preparations continue to build a ballpark for the Oakland Athletics.
Former Bishop Gorman standout Rome Odunze was selected ninth by the Chicago Bears, and former Liberty athlete Troy Fautanu went 20th overall to the Steelers.
The March gaming win was strong — but not as strong as a year ago when casinos had all-time-record slot machine revenue due to a stellar lineup of special events.
Neal Schon of Journey says the Sphere was made for jam bands, but his band would crush it, too.