GPS for the body? Nevada doctors use tech to pinpoint problems
GPS gets most people from point A to point B, but Southern Nevada doctors say the concept applies to a different kind of mapping: surveying and navigating parts of the human body.
Much like dropping a pin on a Google map to guide a trip, physicians can use technology to find far more specific spots than ever before.
At University Medical Center, for instance, doctors can reach deep into the lungs to diagnose cancer — without using a scalpel.
This and other advancements at Las Vegas Valley centers including Sunrise Hospital and Medical Center and Desert Springs Hospital Medical Center often mean patients have shorter stays, quicker overall recovery times and fewer trips back to the doctor.
But they're not cheap, and because of the expense, not all hospitals can afford the technologies that can encourage better patient outcomes. And because of the specialized nature of some of the devices, not all patients will be candidates for them.
Doctors say that as evidence shows the value of new medical technology, the procedures will become more widely available. More people will benefit from them as they learn such treatments are available at a nearby hospital.
GPS FOR YOUR HEART, LUNGS
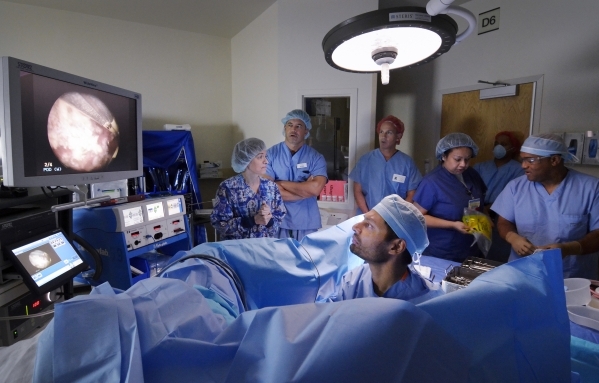
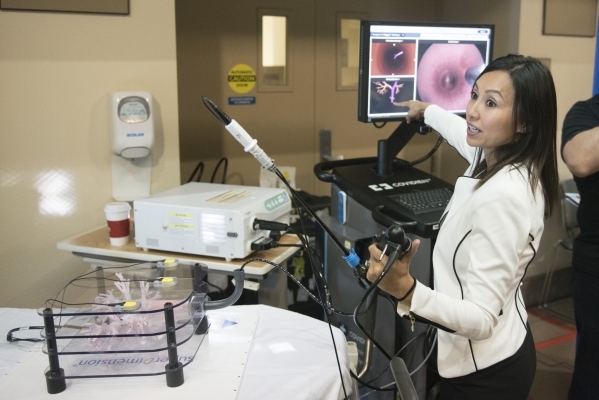
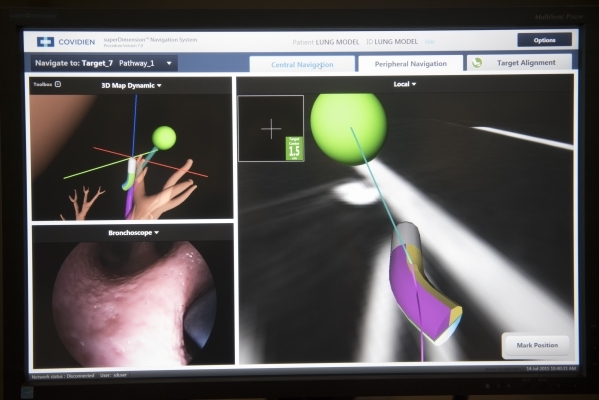
At UMC, new technology is enhancing an old procedure, namely bronchoscopes.
These tubes with scopes examine the throat, larynx, trachea and larger airways, but it stopped there. The hospital's superDimension Electromagnetic Navigation Bronchoscopy system extends the bronchoscope's reach into smaller airways. Catheters can be accurately placed into lesions outside the tube's field of view.
Pulmonologists such as Dr. Hidenobu Shigemitsu can stage suspicious areas for biopsy and treat cancers found in the lungs.
Scans produce 3-D images of the body, giving Shigemitsu and his team a map of the lungs. Other team members include a pathologist who can provide quick results of a biopsy and a thorasic surgeon who can use the data to pinpoint any surgical intervention. Lung GPS minimizes invasiveness and results in early detection of cancers.
"When patients go in for the procedure and wake up, we can tell them exactly what it is, instead of waiting for weeks," Shigemitsu said. "We can make an onsite diagnosis."
The LungGPS technology from Covidien Ltd. costs about $200,000.
UROLOGISTS OFFER BLUE LIGHT SPECIAL
At Sunrise Hospital, a new shade of light is advancing the approach to detecting bladder cancer.
Cystoscopy is an examination of the bladder that scans, collects urine samples and examines the prostate gland. An optic instrument called a cystoscope uses a lighted tip to aid in diagnosing urinary tract and prostate disease.
Doctors also can perform biopsies, the removal of tissue to diagnose malignancies, or remove small stones through a hollow channel in the cystoscope.
When used with the optical imaging drug Cysview, blue light cystoscopy reveals lesions that might not be seen with standard cystoscopy, which works like a flashlight. Cancer, even cells confined to the bladder lining known as carcinoma in situ, demand more blood supply than the surrounding tissues. Blue light cystoscopy with Cysview highlights the cancer with a purple hue on monitors.
The technology also defines the borders of a tumor more precisely during surgery, said Dr. Jayram Krishnan, a Las Vegas urologic surgeon. During a recent procedure, Krishnan alternated between white light and blue light to cut only the amount of tissue necessary to treat his patient.
The technology, developed by medical equipment manufacturer Karl Storz Co., costs just more than $100,000, and Las Vegas urologist Dr. Scott Slavis said the process will be especially beneficial for people with a history of bladder cancer.
"By improving our ability to detect recurrences, we can prevent a lot problems," Slavis said. "We're going to be doing this in an office within two years."
MAGNETIC FIELD WARMS THE HEART
More efficient probes also help doctors at Desert Springs correct irregular heartbeats through procedures known as ablations, the scarring or destruction of tissue in the heart causing the abnormality.
The cardiac muscle pumps blood through the body, but the heart also generates and regulates its rhythm. Electrical impulses pass from one area to another, causing the heart to contract and relax.
Deviations from the heart's normal rhythm, called arrhythmias, can be harmless or life threatening. An ablation involves a long, flexible tube inserted through a vein and threaded into the heart to correct the arrhythmia. Cardiac ablation blocks the abnormal signals.
Patients at Desert Springs can be treated with greater precision, safety and efficiency with Stereotaxis Epoch Solution. The technology offers physicians a computer-controlled, remote magnetic navigation system that helps them guide a magnetic catheter into affected areas of the heart.
"Instead of using a stiff catheter with a handle that allows me to turn, push or pull to get inside the heart, we have a catheter that's floppy. It's tipped like a noodle, a piece of spaghetti," said Dr. Dhiraj Narula, a Las Vegas electrophysiologist, the specialists who diagnose and treat arrhythmias.
That catheter has a magnet that newtworks with Niobe magnets around the patient, and a field is created to allow the doctors to control the procedure remotely.
"Then, we go sit in a control room and manipulate a mouse, pointing in different directions," Narula said. "The advantage is we can manipulate the catheter much more precisely without having to stand right there at the patient's bedside."
The greater level of control and more precise movements improve the safety of the procedure. Patient are at less risk for bleeding or infection, damage to blood vessels, punctures in the heart or damage to heart valves, said Dr. Erik Sirulnick, who like Narula is part of Health Care Partners Cardiology.
"This catheter has no substance to it without the magnetic field," Sirulnick said. "And the amount of force the magnetic field has is not enough to pull it through any tissue. Even the thinnest portions of the heart can't be perforated by it."
The Epoch Solution Niobe ES Robotic Magnetic Navigation System used at Desert Springs typically costs about $2 million from Stereotaxis Inc., Sirulnick said.
Desert Springs was able to buy its nearly new system from the University of Chicago for $1.3 million, said Gretchen Papez, spokeswomen for the Valley Health System.
HOSPITALS BALANCE COSTS, BENEFITS
Hospital officials decide to invest in new techologies based on patient needs, doctor demand, and balancing of the costs and benefits involved. Advances in medical procedures can increase costs in the short term while other technology such as electronic health records, telehealth tools, and staff and management programs cut expenses.
Diagnostic and treatment technologies also can be a selling point for medical schools trying to recruit students.
Dr. Mark Penn, dean of the planned School of Medicine at Roseman University of Health Sciences, said students are drawn to regions where they can learn about the latest advances in medicine from practitioners using the technology.
"Students will get a chance to observe those technologies and be a part of those teams," Penn said. "We will be teaching, just like all the medical schools will, about new technology that's relevant."
Patient outcomes drive innovation in the health care industry because everyone benefits when people get better. That's the goal behind implantable sensors being used by St. Rose Dominican hospitals to monitor the status of heart failure patients.
Dr. Fareed Sheikh is directing the treatments employing the CardioMEMS HF System. Patients take a daily reading, and the information is sent electronically to their doctors who might alter instructions for medications or make other changes to help treat the patient’s heart failure.
The goal of the therapy is to identify problems early and prevent patients from being readmitted to the hospital, which in heart failure can land someone in intensive care on a ventilator.
"I see a lot of heart failure," Sheikh said. "It's just one of the options we have to manage the condition, but it's renewed my energy to embrace the treatment of heart failure."
Contact Steven Moore at smoore@reviewjournal.com or 702-380-4563.