Minimally invasive surgery helps resolve chronic sinusitis
Charlotte Yarbrough couldn’t stand it anymore.
She hadn’t retired to Las Vegas for sleepless nights, headaches, trouble breathing, a reduced sense of smell and taste, facial pain, sneezing or a dripping nose.
A year after she moved here from California in 2011, she learned from doctors that she had developed what thousands of others in the Las Vegas Valley suffer from — allergy-generated chronic sinusitis.
In other words, the delicate membranes in her sinuses — the bony air cavities on each side of the face that filter and humidify air and allow mucus to drain via tiny channels into the nose — had become so inflamed that they caused almost complete blockage of the sinus openings, which can have diameters as small as a coffee stirrer.
Over-the-counter medications didn’t help. Nor did her symptoms resolve with the usual mixture of prescribed medications that include nasal steroid sprays, topical nasal therapies, decongestants, oral steroids and antibiotics.
The prolonged blooming seasons of allergy-inducing plants that researchers say is caused by a warming climate had turned Yarbrough’s planned blissful retirement into a living hell of clogged sinuses and attendant sinus infections.
“I never had allergies a day in my life until after I came to Las Vegas,” she said recently. “I couldn’t sleep anymore. I wasn’t breathing properly. And it was terribly embarrassing the way my one nostril ran all the time.”
Unable to believe there was no solution, she started doing research online.
Thanks to that research, she learned about a procedure known as balloon sinuplasty. Las Vegas eye, ear, nose and throat surgeon Dr. Terrance Kwiatkowski performed it on her in September in his office, and Yarbrough’s clogged sinuses are no more.
“I feel great and it only took about an hour to do,” the 66-year-old Yarbrough said. “I can breathe and sleep again. I’ve been spreading the word in my retirement community. It doesn’t cure allergies but it stops the clogging.
“There really was no pain during the procedure. Just local anesthesia was used. I was awake the whole time. Believe me, if there was pain, you’d hear about it.”
Chronic sinusitis, where medications and treatments don’t help after three months of use, is a huge medical issue in the United States. The National Center for Health Statistics reports that more than 30 million Americans are affected annually at a cost of more than $4.3 billion. Medical economists note that prescription drugs and over-the-counter remedies account for much of the expense but provide little curative benefit for most patients with the condition.
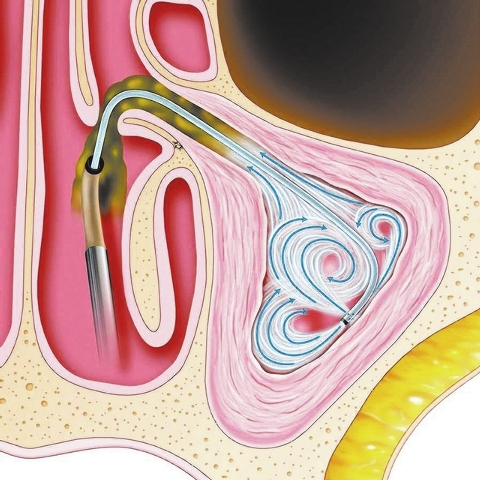
Balloon sinuplasty, hailed as the most exciting advance in the ear, nose and throat field in the past 15 years, uses a catheter and balloon to open and expand blocked sinuses, much like balloon angioplasty does for blocked arteries of the heart.
The procedure, initially cleared by the Food and Drug Administration to treat blocked sinuses in 2005, was largely done in hospitals until the past couple of years. Unlike traditional sinus surgery, it requires no cutting and no removal of bone.
The procedure has a sterling safety record in the hospital — its 0.01 percent risk factor there also holds for office-based procedures. And patients are back to work in two days after the treatment that does not even require an overnight hospital stay. But balloon sinuplasty’s popularity didn’t take off, Kwiatkowski said, until it began to be done more routinely in the office.
More than 350,000 people worldwide have had the procedure done at hospitals, outpatient surgery centers or doctors’ offices, reports Acclarent, a Menlo Park, Calif., maker of balloon sinuplasty instruments.
Many patients didn’t have it done in the hospital because they were leery of hospital procedures, Kwiatkowski said. What happened, he added, is that older friends or relatives of patients could recount sinus surgeries that left them with “12 feet of bloody packing in their nose” and long, painful recoveries. Reports of scar tissue forming after procedures that required even more operations were also plentiful.
“We’ve come a long way since then in all sinus operations, but that perception has held on,” said Kwiatkowski, chief of the minimally invasive sinus treatment program at Sunrise Hospital and Medical Center.
Although some patients still want to have the balloon sinuplasty done in the hospital under general anesthetic, he said the ability to have the procedure in the office using only local anesthesia gave credence to claims of its simplicity and safety.
“I got an anesthetic spray up my nose twice and only felt some pressure, but no real discomfort,” said Yarbrough, who was found to have six sinuses clogged. “I had once before the procedure and once before he unclogged my fifth sinus.”
During balloon sinuplasty, the surgeon inserts a flexible catheter into the patient’s nostril under endoscopic (a small fiber-optic tube) guidance. Using the endoscopic image on a nearby video monitor, along with a CT scan of the patient’s sinuses, the physician guides the tiny catheter into the affected cavity.
Then the doctor inserts a small balloon along the wire inside the catheter. Once the balloon is properly positioned in the blocked area, the doctor inflates it, causing microscopic fractures in the thin bone of the sinus openings that heal in the new, wider, dilated positions. After the widening, the balloon is deflated. As it is removed, the sinuses drain.
The sinuses are often irrigated by the physician to flush out stubborn mucus or other material.
“What I’ve done is move the bone, creating wider openings,” Kwiatkowski said. “What we’ve done is make something that was about the size of the lead in a No. 2 pencil and enlarged it to about the size of the pencil. It’s quite ingenious.”
The effect on Yarbrough, who was able to drive herself home because only a local anesthetic was used, was almost immediate.
“There was very little bleeding and I could breathe again,” she said. “I slept the night of my surgery for 12 hours. I hadn’t slept through in months. For two days I had a little soreness and tenderness and then I was great.”
Although she still has allergies, she can easily treat them with medication. Her sinuses no longer get blocked.
One study of 1,036 balloon sinuplasty patients showed sinus symptoms improved in 96 percent of patients at an average follow-up period of 10 months, with 74 percent freed of sinus infection at an eight-month follow-up. Another study showed significant improvement in patient symptoms out to two years.
Because it is a relatively new procedure, long-term studies are unavailable. But Kwiatkowski said indications are that in as many as 85 percent of cases, the movement of the bone for widening of the sinuses stays in place and will not have to be performed again.
“You can never say never on anything with the human body,” he added.
Kwiatkowski said the surgery is done only on those with chronic sinusitis. He said most people, about 80 percent, can be helped through the usual medicinal care.
He also said that people with polyps or other conditions that help create clogged sinuses aren’t candidates for the pure balloon sinuplasty. But the University of Pennsylvania-trained specialist said he often uses the balloon device to help him “navigate” his way in other more traditional endoscopic surgeries, what he calls “hybrid procedures.”
That’s what he did in removing polyps from 16-year-old Faith Thompson, who had found it almost impossible to breathe through her nose. While he used cutting tools to remove her polyps, he said he used the balloon to help widen sinuses.
“The balloon was just another tool in the toolbox to make sure I got everything just right,” he said of the outpatient procedure done during Thompson’s 2013 Christmas break.
After about a week of recovery, Thompson said she could breathe comfortably for the first time in years.
Yarbrough, whose insurance covered the balloon sinuplasty, said she’s had difficulty explaining the procedure to some of her retired friends.
“There’s this one guy who’s always grouchy because he’s all clogged up,” she said. “He’s been that way for seven years. He’s miserable, but when I described what I had done, that I didn’t even go to the hospital, he said, ‘That’s crazy.’ Some people just don’t want to believe that there’s new things out there that can help us.”
Contact reporter Paul Harasim at pharasim@reviewjournal.com or 702-387-2908.