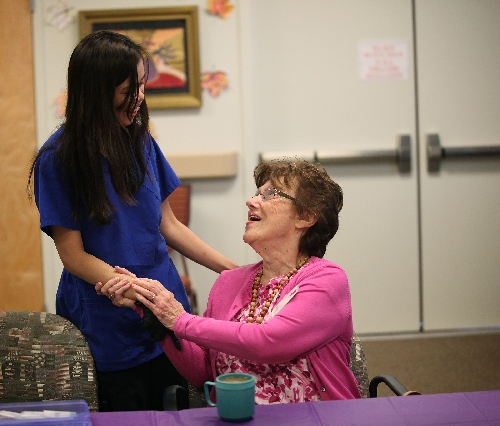
People with Alzheimer’s often face leaving home to receive care
They are Nevadans deep in the throes of Alzheimer's disease, other brain-related conditions or on ventilators, generally low-income Medicaid patients who through no fault of their own have either behavioral problems or can't help themselves.
Given the severity of their condition, families can't care for them at home so they must place them in a nursing facility. Sometimes there aren't enough beds available and Nevada authorities must ship them to out-of-state facilities.
As many as 87 seriously ill men and women - the number fluctuates monthly as Nevada authorities bring patients back as beds become available - are shipped to facilities in Utah, Idaho or even Florida, far from families and friends who love them. About a quarter of the patients have dementia ---- Alzheimer's is the most common form.
"It tears my heart out this happens," says Sally Ramm, the elder rights attorney for the state's Aging and Disability Services Division. "Many have lived here all their lives. Their families don't have any money and they can't travel to see them regularly. They can't help they have Alzheimer's."
The cost of the out-of-state care ---- an average of $255 a day ---- is $57 higher than the equivalent in-state daily rate, according to Elizabeth Aiello, deputy administrator of the state's Division of Health Care Financing and Policy.
Aiello says the state also pays for transportation, generally by plane, or air ambulance, to and from out-of-state facilities. Those costs for dementia patients were not readily available. She says the state does not pay for family visits.
If an Alzheimer's patient dies at an out-of-state home, sometimes the family can't get the remains back, Ramm notes.
"Medicaid doesn't pay to bring back remains, and the family doesn't have money to do it," Ramm explains. "It's just terrible."
Both Ramm and Wendy Simons, chief of the Bureau of Health Care Quality and Compliance that licenses long-term residential facilities in Nevada, say there is a need for more nursing facilities in the state.
They say Nevada must make the "business climate" more attractive to nursing facilities that are staffed and built to handle patients with more complex needs.
Ramm acknowledges that the problem is only going to get worse as baby boomers age.
"I don't think anybody is really ready for what is going to happen," Ramm says.
The Alzheimer's Association reports that about 80 percent of Americans take care of loved ones with the disease in their homes. Others rely on day care, which Nevada Senior Services, for example, offers at $70 a day to the elderly with assorted medical problems. Residential facilities, according to Ramm, can cost more than $5,000 a month.
In Nevada, there are 25 facilities that target the Alzheimer's population with 11 residents or more and 76 facilities with 10 residents or fewer. There are also nine skilled nursing homes for those with severe disease symptoms.
The day-care option for Alzheimer's patients is popular with families who want to care for a relative but need to work.
PROPER CARE
Connie Wilson, 65, has her mother, Elaine Laurain, in the Nevada Senior Services Day Care Center of Henderson. Laurain, 84, was diagnosed with Alzheimer's four years ago.
On the day after the election, Laurain was in an hourlong cognitive stimulation session at the center. Seated next to Ruvo Center psychologist Donna Munic-Miller, who runs the session as part of an outreach program by the Cleveland Clinic, Laurain saw no one else wanted to answer the question posed by the therapist: "Would you like to be president?"
So she did: "I don't think I'm capable of being president. It's a big responsibility that takes years of preparation. I really think anyone would have to be prepared to even think about such a thing."
As the session continued, questions drawn by Munic-Miller from the newspaper were answered by people with memory issues, men and women whose backgrounds ranged from teaching and city planning to construction and homemaking.
After Laurain's daughter heard how her mother interacted in the session, Wilson, who has an at-home business, was both thrilled and saddened.
"That's wonderful. But I wish she could remember what she does during the day," she says. "I ask and most of the time she can't tell me. I know she loves the music, dancing and socializing. Her whole mood has changed since I started taking her to day care. She looks forward to each day now. I was in tears every day before. She just sat home and looked out the window."
The approach to take for people with Alzheimer's, doctors say, differs depending on the severity of symptoms and the progression of the disease. As Munic-Miller pointed out before her class, lost skills aren't regained regardless of approach, but proper management of the disease can make living with it easier, for both the afflicted and the caregiver.
The bottom line for at-home, day-care and residential caregivers essentially follows the same outline. Physical exercise, proper nutrition and socialization are important. So are routine, structured, easily explained daily activities that afford a sense of accomplishment.
As functions are lost, activities should be adapted to allow a person with Alzheimer's to participate. If there are "cues" for desired behavior, such as a label on a drawer for photographs, a person with the disease is more likely to put them back in the right place. A person with Alzheimer's must be kept out of harm's way ---- an unlocked door can be a death sentence to someone who no longer recognizes where his surroundings fit in the scheme of things.
Simons says she advises people thinking of placing loved ones in residential facilities to do a complete inspection, asking plenty of questions. Also ask management for names of those with relatives in the facility so you can contact them, she adds.
"I've found that people with loved ones in facilities are painfully honest," she says.
Simons recommends people contact her office to make sure a facility is licensed; there are people trying to make a quick buck off human tragedy.
Each year, she says, inspectors find about 50 unlicensed facilities have opened for business as care centers. If no one is hurt, the punishment that can be imposed is a $10,000 fine.
Jean Georges didn't want to place her husband, Leonard, in an Alzheimer's residential facility four years ago ---- just the thought of doing so tormented her with guilt ---- but doctors told her that if she wanted to live, she could no longer care for her husband at home.
She had suffered a stress-induced heart attack trying to manage his life, which saw the longtime successful businessman often getting lost and making unreasonable demands as well as unwise financial decisions.
"The most difficult thing I have ever had to do in my life is put my husband in a home," says the 81-year-old Georges, who weeps at the memory.
Today, Georges recommends Prestige Senior Living in Henderson, which can care for 30 people with Alzheimer's in a secure memory care unit. Her husband died there last year at the age of 82. She knows the $5,000 a month price tag is steep.
"They care for the people you love like family, keep them clean and see to it they have good food and so many activities," says Georges. "I know I was fortunate to have Leonard there."
There are times when state-licensed facilities for Alzheimer's patients do not receive such glowing reports. In 2009, the state's Bureau of Health Care Quality and Compliance found that during an inspection of Chancellor Gardens of the Lakes, at 2620 Lake Sahara Drive, many - perhaps all - of the 139 patients had gone without their medications for weeks. The facility's former wellness director told inspectors that she knew caregivers were "throwing the medications away" ---- including diabetes medications ---- "because they did not have the time" to administer them.
That year a patient from the facility also went missing and was found five days later in a diabetic coma. He died.
The facility was fined more than $100,000 and admissions were banned for months.
Len Arnold, the new executive director of the facility, says he's brought in a new medical team.
"We got rid of the bad people," he says. "We now receive an 'A' grade on inspections and advertise that."
PRESCRIBING DRUGS
Congress has also been looking at how facilities care for Alzheimer's patients. Last year a Senate committee heard testimony from relatives of patients and medical professionals who felt that too many individuals in facilities were being overprescribed dangerous anti-psychotic drugs to keep them compliant. Proposed legislation would allow federal authorities to develop a protocol for obtaining informed consent before administering anti-psychotics.
Studies have shown that use of the drugs puts an elderly person at a higher risk of death. Those on the drugs often have what are referred to as a "zombie look."
"I saw that look when I inspected some facilities for my mother, and it worried me," Connie Wilson says.
Dr. Charles Bernick, a neurologist and associate medical director of the Cleveland Clinic Lou Ruvo Center for Brain Health, says overprescribing anti-psychotics to keep patients sedated "can be a problem."
If Jeff Klein, the CEO and president of the two adult day-care centers run by Nevada Senior Services ---- one in Henderson and one in Las Vegas ---- had his way, there would be few Alzheimer's patients in residential facilities.
"I view it as a failure whenever any of our Alzheimer clients have to go to a facility," he says. "I feel like we haven't helped out the caregiver at home enough."
Klein says he's sure those with the disease have a better quality of life when they still live around relatives and can be taken to a day-care facility where they are stimulated by socialization, exercise and classes in the arts and humanities.
"We make sure people get up and move as much as possible, make sure they're doing meaningful things," he says.
He notes that trained staffers at the center dispense drugs prescribed by a doctor and, if need be, keep their clients diapered. Clients also receive nutritious meals. There are stress-relieving classes for the caregivers as well.
Few people, Klein says, have to pay the $70 daily rate because he finds grants to help defray costs.
Former first lady Rosalynn Carter, founder of an institute bearing her name at Georgia Southwestern University, was so impressed with Klein's program that Nevada Senior Services was one of five sites in the country awarded a $150,000 grant.
Ernest Williams, an 81-year-old Korean War veteran, showed up the other night at Klein's day-care center in Las Vegas to pick up his wife, 76-year-old Inas Williams. He had brought her early in the morning and was picking her up in the darkness of the early evening. She has had Alzheimer's for nearly six years and Williams took care of nearly all her needs during that time.
"She can't do anything for herself anymore," he says. "I've fed and bathed her because I love her. But it became too much, and I found this place. I've got hospice coming into the home now, too.
"I wish she could take advantage of all they have here. But I think she enjoys being around all these people and it gives me a little rest. They keep her nice and clean like she's family," he says.
"I'll tell you why this place works: It's because these people, everyone of them who works here, has a heart as big as a bushel basket."
Contact reporter Paul Harasim at pharasim@reviewjournal.com or 702-387-2908.
Alzheimer’s disease: A Rising Storm
The Review-Journal presents a series about Alzheimer’s disease and its impact on society, today and potentially in the future.
• An overview outlining the prevalence of the disease and efforts by families to cope with it and by researchers to treat and cure it
• The financial impact of the disease on families and society
• Challenges for the 80 percent of Americans who choose to care for their loved ones with Alzheimer’s disease at home
• Alternative forms of care, from day care to assisted living and nursing homes
Upcoming:
Tuesday
• Identification and treatment of Alzheimer’s disease
Wednesday
• Debate about the benefits of testing for Alzheimer’s
Thursday
• The state of Alzheimer’s research and what is needed in the future
FINDING HELP
These are local organizations that help people with Alzheimer’s disease and their families. Some accept volunteers.
Alzheimer’s Association, Desert Southwest Chapter, Southern Nevada Region
The association offers general information, support groups, educational programs, referrals and opportunities to volunteer.
Address: 5190 S. Valley View Blvd., Suite 104, Las Vegas, NV 89118
Phone: 702-248-2770
24-hour Helpline: 800-272-3900, operates seven days a week, in 140 languages
Cleveland Clinic Lou Ruvo Center for Brain Health
Address: 888 W. Bonneville Ave., Las Vegas, NV 89106
Phone: 702-331-7054
Appointments: 702-483-6000, Option 2
Information about services and programs for caregivers and families: 702-483-6023
Information about enrolling in a clinical trial: 702-685-7073 or brainhealth@ccf.org
Donations: Cleveland Clinic Lou Ruvo Center for Brain Health Philanthropy Institute, 702-331-7052
Volunteer: 702-331-7046
Keep Memory Alive: 702-263-9797