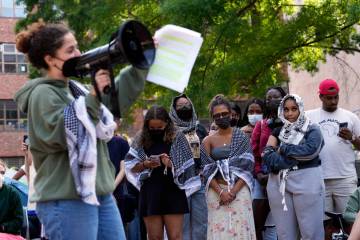Hepatitis C patients wait, hope
Even when exhausted from treatment with interferon, a potent substance sometimes capable of beating back hepatitis C, 61-year-old Gwendolyn Martin has to take medication to help her sleep.
"Having hepatitis C really plays games with your mind," she said.
When Martin tries to nod off naturally, she envisions the virus that public health officials say she picked up at the Endoscopy Center of Southern Nevada snaking through her, eating away at her insides.
Or she imagines her husband of 43 years, the man she calls her soul mate, infected from loving intimacy.
Or she can see herself cutting her finger while making dinner and her tainted blood infecting her family.
Yet those nightmares remain largely only that, for they concern parts of her life that the virus has stolen from her.
"I go for counseling and hope things get better," Martin said as she sat next to her husband, Lovey, in the law offices of Nia Killebrew, an attorney representing 22 former patients who believe their procedures at Dr. Dipak Desai's clinics led to positive hepatitis C tests.
"She never laughs anymore," said Lovey Martin, a semiretired vice president of an information technology firm.
For nearly a year ending in January, Gwendolyn Martin also dealt with interferon treatment, which carries a number of side effects.
She got through the fever, chills, headache, body aches, fatigue, decreased appetite, weight loss, hair loss, rashes, decreased white blood cells and platelets, anxiety, depression, difficulty concentrating and impaired memory.
Martin won't know until April whether the therapy lessened her chances of suffering from the potentially fatal liver disease.
But on the first anniversary of the largest notification of its kind in the nation's history -- a year ago public health officials urged 50,000 patients of clinics owned by Desai to get tested for hepatitis and HIV -- Martin says she does know this:
"We can't forget what happened. If we do, it will happen again."
On Feb. 27, 2008, in a news conference held at the offices of the Southern Nevada Health District, health officials revealed that authorities investigating a cluster of hepatitis C cases had observed nurses at the Endoscopy Center's Shadow Lane clinic reusing syringes in a manner that contaminated vials of medication and, they believe, infected patients.
This practice, according to city investigators, was done at the direction of Desai and other administrators.
Six of the cases, including Martin's, were linked to procedures on Sept. 21, 2007.
Martin didn't find out she had the disease, however, until two months later when she went to the emergency room at MountainView Hospital with severe flulike symptoms.
Health officials told her the news of her link to the outbreak prior to their public announcement.
A total of nine cases have been linked to two Desai clinics, and health officials have listed an additional 105 cases as "possibly related."
The criminal investigation of the outbreak shows that the wheels of justice do grind slowly, said Capt. Al Salinas, head of the Metropolitan Police Department's organized crime unit.
But he said it is important that people realize they continue to grind.
"I believe we'll have a case ready to present to the district attorney in two or three months," he said.
Deputy District Attorney Scott Mitchell has said he believes felony grand jury indictments could be returned for criminal medical negligence or battery with substantial bodily harm in connection with the case.
Salinas said the two police investigators and a financial analyst working the case continue to talk with witnesses and "have found it terribly time consuming" to examine 128 computers found at Desai's clinics.
Messages on the computers could reveal in more depth how the clinics worked, Salinas said.
Jim DiFiore, manager of the city's business services decision, suspended Desai's business license in the wake of the outbreak.
At that time, DiFiore said in a letter to the clinic's owners that health investigators told him that Desai ordered his nurses to reuse syringes and reuse single-dose vials of medication when administering anesthesia to patients who received endoscopic procedures.
Desai did it to save money, DiFiore said.
Salinas said police initially found witnesses in the case to be uncooperative.
Many feared losing the medical licenses that put bread on the table. Rather than give a statement to police, he said, they opted for being subpoenaed before a grand jury, a process which takes far more time.
"Now people are being more cooperative, because they're finally realizing they have to look out for themselves," DiFiore said. "Now that we have information from computers, they better cooperate all they can."
It is still unclear whether Desai could delay the case.
A hearing officer for the Nevada State Board of Medical Examiners recently ruled that Desai, who is facing a medical malpractice complaint, must undergo an independent physical examination before March 30 to determine if he's still suffering residual effects of a July stroke.
Medical records submitted from his legal team dating back to September continue to show his medical condition has not improved.
But Mitchell said records seen by a medical expert working with law enforcement officials indicate that Desai would have no problem participating in a criminal defense.
Two colleagues of Desai, Drs. Eladio Carrera and Clifford Carrol, face disciplinary hearings before the medical board this summer in connection with the hepatitis outbreak.
Debra Scott, executive director of the Nevada State Board of Nursing, said the regulatory board is still conducting its investigation.
Six nurse anesthetists who worked at the Shadow Lane facility voluntarily relinquished their licenses early last year. Disciplinary hearings have not been scheduled for those nurses.
The nursing board also has filed complaints against 22 other nurses who worked at Desai's facilities, largely for a "failure to report" information critical to patient safety to regulatory agencies.
Officials have said the information was not reported to the appropriate regulatory agencies out of fear of retaliation, especially loss of employment.
In an effort to prevent this from happening in the future, Nevada lawmakers have introduced Assembly Bill 10. If passed, the bill would prohibit retaliation against nurses and nursing assistants for reporting to authorities information relating to patient safety.
The FBI, IRS and state attorney general's office also continue to investigate. They declined last week to discuss the status of any investigations.
Mitchell has said he believes federal and state authorities, who meet regularly with local investigators, do not want to bring cases of billing fraud in connection with Desai's clinics until any local criminal prosecutions are over.
What happened in Las Vegas is having ramifications beyond Nevada's borders.
As a result of the outbreak, officials with the Centers for Disease Control and Prevention have said Nevada soon will be the pilot site of a national effort to educate patients and medical providers about injection safety standards.
That makes good sense to Gwendolyn Martin, who recently lost her job as an administrative assistant at a Las Vegas architectural firm and now has new insurance worries to deal with.
But she thinks any effort must include reminding medical providers of their oaths.
"Greed is not in any oath that I know of," she said.
Review-Journal writer Annette Wells contributed to this report. Contact reporter Paul Harasim at pharasim @reviewjournal.com or 702-387-2908.