Hydrocodone reclassification compounds some patients’ pain
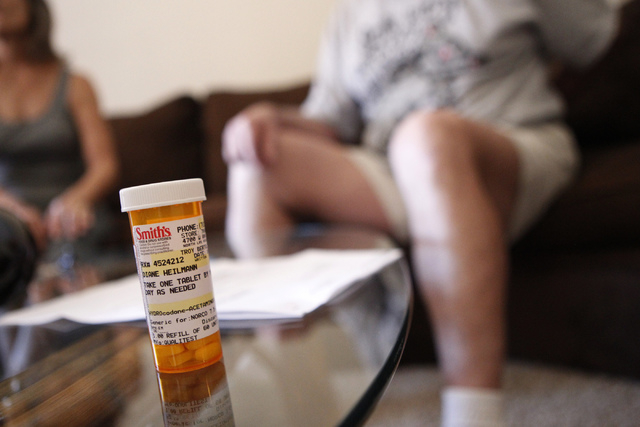
Minutes into a conversation, Diane Heilmann rearranges the pillows on her sofa and changes positions gingerly. She’s not concerned about appearances. She’s following medical advice.
Heilmann, who suffers from rheumatoid arthritis, knows the other techniques that can ease her pain: rest, alternating heat and cold, pacing activities to reduce stress, massage. Nothing, however, can control her symptoms like medication, often the only relief for arthritis patients.
“If I don’t take my medications, I live in pain,” she said.
That’s why the 69-year-old former Bullhead City, Ariz., city clerk and her husband, Brian, were stunned by new rules for her primary pain medication, Norco, a combination of hydrocodone, an opioid pain reliever, and acetaminophen, Tylenol’s active ingredient.
Hydrocodone combination products often are prescribed for patients with painful chronic diseases. Some patients worry they might have trouble filling their prescriptions because of the new rules, which took effect Oct. 6. Some patients are learning of the change from their pharmacists.
The Drug Enforcement Administration has reclassified hydrocodone combination products from schedule III to schedule II under the Controlled Substances Act, which will more tightly restrict access. For example, patients seeking Vicodin, Lortab or Norco generally must present a written prescription to receive the drug, and doctors will no longer be able to call in a prescription to the pharmacy in most instances.
The biggest change for the Heilmanns is the requirement that she see her doctor every month instead of every three months. Brian Heilmann considers the added visits not just unnecessary but an activity that could complicate his wife’s condition. Movement is one of the factors that aggravates Diane Heilmann’s arthritis.
The regulation is a response to widespread misuse of prescription painkillers, but some patients, doctors and pharmacists complain the new rules restrict access indiscriminately.
While acknowledging the added hardship for some patients, Dr. Larry Pinson, Nevada Board of Pharmacy’s executive director, said some action was needed because of the increase in abuse and adverse events related to opioid painkillers. Ninety-nine percent of the hydrocodone produced worldwide is consumed in the United States, Pinson said.
More people in Southern Nevada die from prescription drug overdoses than methamphetamine, heroin and cocaine combined, according to Kent Bitsko of the High Intensity Drug Trafficking Areas program. Bitsko’s task force provides assistance to local law enforcement agencies because Southern Nevada is a significant drug-trafficking region of the United States.
Prescription medications nearly have overtaken marijuana as the gateway drug for people who become addicts, Bitsko said.
Methamphetamine is the top narcotics concern for law enforcement, Bitsko said, but abuse of prescription painkillers is second. More oversight of prescription medications makes acquiring those drugs more difficult, and many abusers eventually seek alternatives.
“When they can no longer get hydrocodone, they turn to heroin,” Bitsko said.
At Nevada Pain Specialists, patients prescribed hydrocodone already were required to see a doctor once a month for patient safety. Dr. Steve Gephardt said patients at his company’s two clinics in Southern Nevada often have prescriptions for tranquilizers or antihistamines that put them at risk for adverse effects.
Gephardt said doctors at his clinics also use the state prescription monitoring program, a pharmacy board database that stores information on federally controlled substances. All of a patient’s prescriptions are stored in that database. The program, which doctors are not required to consult, can identify when patients might be trying to acquire more medications than they should have for their illnesses.
“As a prescriber, the biggest concern we have is patients ‘doctor shopping,’ patients getting medications from multiple physicians and then selling them,” he said.
Coincidentally, the new rules took effect during Breast Cancer Awareness Month, and some cancer patients will be affected by the changes. People with cancer often suffer from such intractable pain that they are prescribed schedule II medications, said Dr. James Sanchez, an oncologist at Comprehensive Cancer Centers of Nevada. Sanchez worries the new rules will make some pharmacists more “drug shy,” or unwilling to fill a prescription because it falls outside the recommended guidelines. Doctors might prescribe pain medications for some cancer patients outside those guidelines.
Cancer often requires the use of pain medications long term, and patients don’t need the added indignity of withholding medications because of suspicions over misuse, Sanchez said.
“We have patients that have long-standing needs for pain medication,” he said. “They’re just living longer even though they have such a serious disease. If you’re going to treat pain, you should treat it to a level that’s productive.”
The Heilmanns know they are fortunate. Their pensions and insurance can cover any added costs associated with more visits to the doctor. Brian Heilmann, 62, also suffers from chronic pain from clashes during his days as a police officer and prison guard. He has had numerous surgeries for back and knee problems, but he takes oxycodone, which already was a class II medication.
Diane Heilmann remembers her days as a city clerk taking calls from senior citizens worried about rising costs, and she wonders how people on fixed incomes will adjust to seeing a doctor 12 times a year instead of four.
“They might not be able to go to the doctor once per month,” she said.
Brian Heilmann said he dreads the added doctor visits because of the inconvenience and cost, such as co-pays, associated with going to the doctor, and he empathizes with those who might not be able to afford the changes.
“I’m lucky. I have good insurance from Blue Cross/Blue Shield,” he said. “We’ll just have to wait and see what happens.”
Contact Steven Moore at smoore@reviewjournal.com or 702-380-4563.

Did you know …
Hydrocodone-combination products contain hydrocodone (a Schedule II drug) and other ingredients like acetaminophen.
Rules that apply to Schedule II drugs are more strict than rules for Schedule III drugs. Among the differences:
You must see a doctor to get a prescription refill for a Schedule II drug, while doctors can call in prescriptions for Schedule III drugs.
The Drug Enforcement Agency says almost 7 million Americans abuse prescription drugs that contain controlled substances. More people die from overdoses than from auto accidents.
Schedule II drugs are substances with accepted medical uses that have a high potential for harm and abuse, according the Controlled Substances Act.
If Schedule II means more rules, what’s a Schedule I drug? Illegal drugs fall under the Schedule I category. Heroin, Ecstacy and Quaaludes are examples. See these lists:
Schedule I drugs
Schedule II drugs
Schedule III drugs