Las Vegas fertility doctor helps people become parents
Joy.
How wondrous it is to feel that all is right in the world, when your tears aren’t fueled by sadness, when the butterflies in your stomach aren’t caused by fear, when that spring in your step feels as though it will catapult you into a life bathed only in goodness.
When I’ve talked over the years to parents whose babies were born with the help of fertility specialist Dr. Geoffrey Sher — couples including Andrew and Heather Lynch, the parents of 5-month-old twins Benson and Anakin — I see the joy in their faces and hear it in their voices as I remember how I felt when my own children were born, when only love filled my soul.
Like most people, my wife and I were able to have children without assistance. Not everyone who wants children is as fortunate — nearly 1 in 6 couples worldwide are unable to naturally conceive and have a baby carried to term.
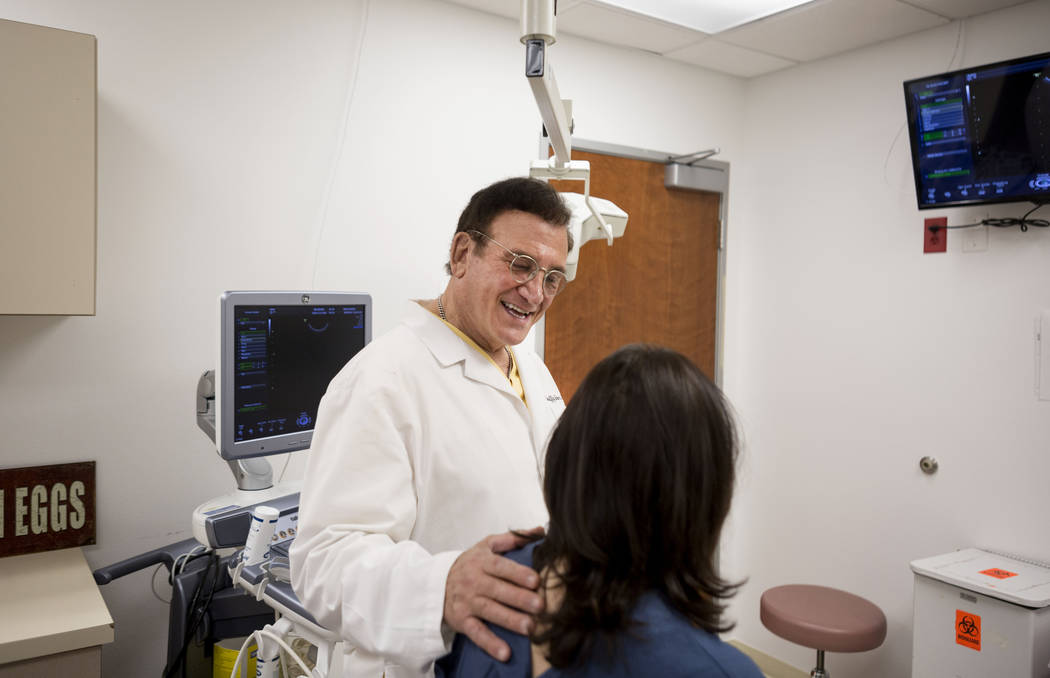
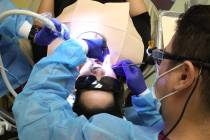
For three decades Sher, 74, has helped people with fertility problems. Because of his expertise, he’s been influential in the births of more than 18,000 children, including Aaron and Megan Barborka’s 14-month-old twins, Henry and Lorea. At one time, Sher had a nationwide network of eight fertility clinics, with doctors who had trained under him. In 2015, he sold his ownership in all but the Las Vegas clinic.
Beating the odds
Before going to Sher, more than half of his patients have been to other doctors without success. Karmann Wennerlind had a half dozen miscarriages before she and her husband, Ryan, found Sher. They now are the parents of 3-year-old Kai and 1-year-old Kamryn.
When Sher told me recently that he would retire next year to travel — he’s giving months of advance notice because 75 percent of his patients are either from out of state or out of the country while others have frozen embryos and eggs stored at his clinic — one thought keep running through my head.
I hope he’s trained his younger colleagues well.
His patients share that hope.
“I don’t know how the fertility world will be without him,” said Karmann Wennerlind, who overcame her body’s “killer cells” to conceive. “He’s impacted the lives of so many women and families. He’s thinks outside the box to find problems.”
A pioneer in IVF in U.S.
A native of South Africa, Sher trained in England with Dr. Patrick Steptoe and Robert Edwards, recipient of the 2010 Nobel Prize for Physiology or Medicine. Edwards’ work led to the first “test tube,” or in vitro fertilization (IVF), baby, where an egg is fertilized by sperm in a test tube or elsewhere outside the body.
Once an embryo or embryos form, they are placed in a woman’s uterus.
Sher opened the first private IVF program in the United States in 1982. He left California to open his Las Vegas clinic 20 years ago. His research has resulted in more than a dozen “firsts” that have made fertility treatments more successful.
Both Oprah’s show and ABC’s “Nightline” have called him for insight into fertility medicine. Netflix carries a documentary by Oscar-nominated director Amanda Mitchell, “Vegas Baby,” that follows people trying to win free treatment by Sher.
His patients — their average age is 37½ and more than 70 percent have failed IVFs elsewhere — often travel from afar because of complex problems and repeated failures.
Sher knows that science has yet to unlock all the mysteries of the human body, so success rates of 50 percent are considered excellent. It is why he tells his patients to pray, the reason he always shares with them this turn of phrase, “Man proposes, but God disposes.”
Sher says that direct translation from “The Imitation of Christ,” a work of devotion written in Latin by Thomas à Kempis, is a reminder that people can make plans, but God determines how things will turn out.
Worth the struggle
As I sat in the living room of Andrew and Heather Lynch, it was obvious as they played with and bottle fed their twins, that life has turned out as they hoped and prayed.
They cooed as they told their little ones how much they loved them.
It took six years and about $36,000 — a fertility specialist who was unsuccessful and Sher both charged about the same — to find a way to deal with a disorder in Heather’s uterus. Most of the treatment is not covered by insurance.
For a UPS driver and a stay-at-home mom, that bill is not easy to handle.
“It’s been worth it,” Heather said. “We’ve always wanted a family and now we have it. It was hard on us getting here, very, very emotional, but we made it. Now we can enjoy it.”
It took nearly five years and a dose of good luck for the Barborkas to get pregnant.
After a less invasive fertility treatment with one doctor didn’t work, they won a raffle in 2015 for free a IVF cycle from Sher, which quickly turned out to be successful.
Aaron Barborka, now in dental school, said he and his wife believe that families are what bring the most joy in life.
“The connection with kids is something that you don’t have in any other relationship,” he said. “Our marriage is special. But to rear kids, teach them, watch them grow, it’s something we both have longed for ever since we were married. I can’t imagine anything that could bring more joy.”
Amen.
Paul Harasim’s column runs Monday in Health. Contact him at pharasim@reviewjournal.com or 702-387-5273. Follow @paulharasim on Twitter.
Dr. Sher's accomplishments
■ 1982: First to recommend and publish the benefits of the exclusive use of injectable fertility drugs (gonadotropins) to stimulate the woman's ovaries for in vitro fertilization, or IVF, where an egg is fertilized by sperm in a test tube or elsewhere outside the body. Prior to that, oral fertility drugs had been preferred, with much lower success rates being reported.
■ 1983: First to introduce intrauterine (artificial) insemination (IUI) of washed/enhanced sperm for treating certain forms of infertility.
■ 1989: First to report on the ultrasound appearance and thickness of the uterine lining (endometrium) as a predictor of whether the embryo is likely to implant successfully following IVF.
■ 1993: First to introduce the technique of "prolonged coasting" to treat women in whom the use of fertility drugs for IVF resulted in severe "overstimulation," placing them at risk of life-threatening complications, and thus virtually eliminating such risk.
■ 1994: Among the first to identify and treat immunologic abnormalities that prevent implantation of the embryo.
■ 1997: First to introduce vaginal Viagra suppositories to improve uterine blood flow and enhance hormonal thickness of the uterine lining.
■ 1998: First to recommend the selective use of a blood product (intravenous gammaglobulin ) for treating certain forms of embryo immunologic implantation dysfunction in IVF.
■ 2000: Introduced a protocol for ovarian stimulation — the agonist/antagonist conversion protocol — to improve egg/embryo quality in response to fertility drug stimulation.
■ 2003: First to measure a genetic marker and use it to identify the "best individual embryos" (ones most likely to implant and produce a viable pregnancy) for transfer to the uterus.
■ 2005: First to show that biopsying embryos to assess their full chromosome integrity (using pre-implantation genetic screening — PGS) can identify those embryos most likely to be "competent" to propagate viable, healthy babies and a much lower risk of miscarriage.
■ 2007: First to show, by using PGS, that an embryo resulting from fertilization of an egg that has all of its chromosomes present has a much improved ability to implant successfully and produce a normal baby.
■ 2008: First to apply egg biopsy and PGS to the select chromosomally normal eggs for freezing and banking (fertility preservation), leading to a four- to six-fold improvement in the birth rate per frozen egg.
■ 2014: Among the first to report that some embryos that have an abnormal chromosome component have the ability to self-correct in the uterus and proceed to propagate healthy babies.