Value lacking in LV health care
Las Vegas ranked poorly in a national study evaluating cities for the value of care their hospitals give patients, and the report's authors suggest managed-care dynamics and the uninsured might be behind the city's low rating.
Las Vegas placed No. 82 out of the country's 100 biggest markets in an analysis that weighed hospitals' affordability and efficiency against quality of care and patient satisfaction.
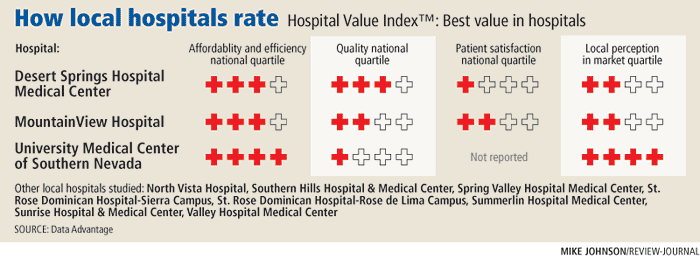
The study, from Kentucky-based health care information firm Data Advantage, singled out three area hospitals for providing the best value of care for patients. Desert Springs Hospital Medical Center, which belongs to United Health Services of Pennsylvania, scored highest overall, pulling in strong marks for affordability and efficiency and quality. MountainView Hospital merited solid reviews in affordability and efficiency, while University Medical Center ranked well in measures of affordability and efficiency and local perception of the hospital's services.
Hal Andrews, chief executive officer of Data Advantage, said the analysis doesn't indict the quality of care available here -- hospitals in Las Vegas "do a good job on quality," he said -- but the statistics show the city's acute-care centers could improve the balance between their costs and the prices they charge for care.
Rick Plummer, a spokesman for University Medical Center, said the hospital appreciates open dialog about quality, efficiency and other measures, but it looks to more direct gauges of service.
"You can't look at these types of studies enough because of the importance of them," Plummer said. "But at the end of the day, the only study we care about is our patients and the care they receive."
Plummer said UMC officials assess their value and quality mostly through data from the Centers for Medicare & Medicaid Services, rather than from figures found in research firms' studies.
"Quality in health care is a destination," he said. "We're always striving to get better. We're always looking for ways to tweak and fine-tune and run things more efficiently. Health care is a constant work in progress, and that's a good thing."
Sunrise Health officials said they wouldn't comment on the study's results until they had the opportunity to review the report in-depth.
Officials with Universal Health's local five-hospital operation and representatives of St. Rose Dominican Hospitals didn't comment before press time.
To develop its rankings, Data Advantage researched numbers from the Centers for Medicare & Medicaid Services, the National Research Healthcare Market Guide and the Joint Commission on Accreditation of Healthcare Organizations. They looked at the quality of care, the prices hospitals charge, patient experiences and reputations.
In all the numbers-crunching, lower-ranked markets seemed to share two traits: They featured managed-care insurance markets with high penetration and stiff competition, and they contained more uninsured patients than average. Nevada followed the trends; its managed-care penetration runs at roughly 60 percent, compared with a national average below 50 percent, while its share of uninsured patients totals about 21 percent, compared with 15 percent nationally.
Andrews said the correlation between lower hospital care values and competitive managed-care climates surprised him, and he plans to study the issue further. His theory: "End-of-contract showdowns" and "fierce managed-care fights," like the recent battle between insurer Sierra Health Services and the four-hospital Sunrise Health system, put hospitals into a "defense posture" that makes it tougher to focus on boosting efficiency and reining in prices.
"Hospital value is lower for the purchaser, whether it's a consumer or an employee, in competitive managed-care markets," Andrews said. "That's counterintuitive to everything we thought about managed care."
It's easier to understand how uninsured patients contribute to low value, Andrews said. Costs among patients who don't pay for care shift onto the hospital bills of consumers with insurance or other means for covering their tabs.
The factors could explain why the list of top markets for hospital values are mostly back East, while Western cities dominate the ranks of lower-value markets. Managed-care competition and lack of insurance are far more common out West than they are on the East Coast, Andrews said. California houses seven of the 10 worst markets for value. Among the markets rating below Las Vegas: Houston; San Antonio; Phoenix; Los Angeles; Sacramento, Calif.; Albuquerque, N.M.; San Francisco; Denver; and Tacoma, Wash.
Plummer agreed that managed care and indigent patients could make a difference in the value hospitals provide.
"Managed-care companies are requesting lower and lower reimbursement rates, and someone has to pay, and the cost of medicine goes up for every indigent patient," Plummer said. "If you have an indigent patient who comes into the ER, the next five patients pay for that. Their costs go up."
Improving value won't be easy, because hospitals "are already doing everything they can in the face of all the pressures they're under," Andrews said.
Consumers and employers, on the other hand, have some power to effect change.
Andrews urged people who pay for hospital services to vote with their dollars, and reward value-oriented hospitals by giving them more business.
"Employers need to start holding hospitals accountable for delivering value both good and bad," he said. "There's not really a correlation between good value and which hospitals reap the benefits. Employers, for the benefit of employees and other consumers, need to start recognizing hospitals that do a good job."
Contact reporter Jennifer Robison at jrobison@reviewjournal.com or 702-380-4512.
MARKETS FOR HOSPITAL VALUE
Data Advantage, a health information company based in Kentucky, ranked the nation's 100 biggest cities in the value of care their hospitals provide to patients. Here are the company's top and bottom 10 markets for value:
1. Buffalo-Niagara Falls, N.Y.
2. Rochester, N.Y.
3. Springfield, Mass.
4. Essex Co., Mass.
5. Syracuse, N.Y.
6. Grand Rapids-Wyoming, Mich.
7. Pittsburgh
8. Knoxville, Tenn.
9. Cambridge-Newton-Framingham, Mass.
10. Charlotte-Gastonia-Concord, N.C.-S.C.
82. Las Vegas
91. Los Angeles-Long Beach-Glendale, Calif.
92. Sacramento-Arden-Arcade-Roseville, Calif.
93. Stockton, Calif.
94. Albuquerque, N.M.
95. San Francisco-San Mateo-Redwood City, Calif.
96. Denver-Aurora, Colo.
97. Oakland-Fremont-Hayward, Calif.
98. Oxnard-Thousand Oaks-Ventura, Calif.
99. San Jose-Sunnyvale-Santa Clara, Calif.
100. Tacoma, Wash.
See the whole list online at www.hospitalvalueindex.com
SOURCE: Data Advantage