Nevada may be near peak of COVID-19 cases, but 2nd wave feared
Although Nevada and Clark County might be near a peak in COVID-19 cases — or possibly even have passed it — local health authorities say that doesn’t mean the worst is over.
After sharp increases, new cases have shown signs of slowing in recent days, while some prominent forecasting models suggest that the state may have passed the outbreak’s peak.
But Southern Nevada Health District officials say they are skeptical of such projections based on what they’re seeing on the ground.
“In looking at our data, it doesn’t appear that we’ve reached our peak,” Mike Johnson, director of the Southern Nevada Health District’s Community Health Division, said during a telebriefing with reporters on Friday.
“Even if we see a leveling off of cases, we don’t want people to think they’re home free now,” added Dr. Vit Kraushaar, medical investigator for the district.
The health district officials did not speak directly to whether Southern Nevada could meet White House-prescribed thresholds for “opening up” states and easing restrictions, but cautioned against moving too soon to end social distancing and other emergency measures in the state.
Nearing the peak?
In guidelines released Thursday to ‘open up” America in a phased approach, the White House coronavirus task force issued general criteria to be met that begin with a “downward trajectory of documented cases.”
After sharp increases in late March, the statewide increase in new cases have leveled off and even declined, with the greatest number of news cases — 258 — on March 29, followed by 231 on April 7, 228 on April 3, and 203 on April 16, according to state data. As of late Friday, there had been 3,524 cases of COVID-19 in Nevada, and 151 deaths.
Modeling by the University of Washington’s Institute for Health Metrics and Evaluation, which is often referenced by the White House’s task force, indicates Nevada passed its highest daily death toll earlier this month at 26, with peak hospital resource use forecast to occur sometime between April 7 and Saturday.
But the forecasts have varied widely among models, and estimates often have changed within individual models as newer data has been incorporated. However, an official in Washoe County on Friday pointed to a model by Los Alamos National Laboratory that also indicated there was an 80 percent chance that Nevada already had seen its peak infection rate.
Las Vegas Valley hospitals, including University Medical Center, said they believe they’re at or near the peak in terms of COVID-19 cases.
“Our internal data does not show we have peaked yet, but that we are getting much, much closer,” said Dr. Joe Corcoran, chief medical officer of HCA Healthcare’s Far West Division. “Based on what we are experiencing at Sunrise, MountainView and Southern Hills hospitals, our number of COVID cases is still rising but the rate of growth is now in low single digits and slowing almost daily.”
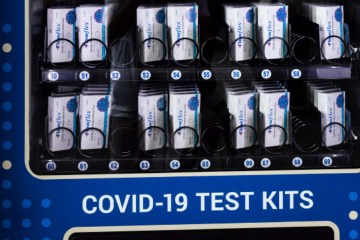
Another provision of the recovering guidelines is a “robust testing program for at-risk health workers,” something that is coming closer to fruition now that hospitals are gaining the capability for rapid testing, officials said.
Another requires that hospitals be capable of treating all patients “without crisis care.”
Hospital staff have said that while there are treating many COVID-19 patients, their facilities have not been been overwhelmed and they have not needed to go into crisis mode.
State and county data support this.
The state’s nvhealthresponse.nv.gov website reported that 61 percent of hospital beds and 70 percent of intensive care unit beds were in use, along with 39 percent of ventilators. In Clark County, 65 percent hospital beds and 77 percent of ICU beds were occupied, and 44 percent of ventilators were in use.
But health-care providers remain watchful in case the pace of new infections and hospitalizations pick up again.
Gretchen Papez, a spokeswoman for the Valley Hospital System, said that while they hope the peak is behind them, “We are continuing to maintain all preparations for a surge.”
‘Ugly fact’
That concern is not without basis.
With a pandemic, there may also be more than one surge.
Kraushaar described the COVID-19 pandemic as a “once in 100 years situation,” and noted that with the Spanish flu pandemic of 1918, the second wave of illness was more severe than the first.
He urged caution in easing restrictions, as did Karen Duus, an associate professor in microbiology and immunology at Touro University Nevada in Henderson
“The advantage of flattening the cure was primarily to keep our hospitals and our personnel from getting overwhelmed,” Duus said. “It doesn’t change the ugly fact that every single one of us is more or less susceptible to this virus because no one has seen it before.”
People are likely to continue getting sick “until enough of the population has been infected so that herd immunity kicks in,” she said. Herd immunity refers to when enough people have developed resistance to the disease, either through being infected or through immunization, that it stops the disease from spreading.
But the novel coronavirus is still so new that it’s not even clear whether people who have been infected with the disease will develop immunity, and if they do, how long it would last.
“I think, basically, as long as we’re all staying at home and not mingling, we’re all good,” said Duus, whose research has focused on viruses. “The problem is, if we all go back to our usual ways, the virus can be transmitted again.
“If we’re going to go back to a somewhat normal situation, we’re going to have to make some hard choices.”
Hard choices, she said, such as wearing masks any time we venture outside our homes and when possible, staying away from other people.
“I’m as eager as the next person to get out of my house and back to school and see my students’ smiling faces. … That doesn’t mean that I’m going to be eager to walk into a classroom of 180 medical students,” she said.
Duus envisions when restrictions finally do ease, that she might be teaching online classes along with some “very, very small classes with lots of space.”
Contact Mary Hynes at mhynes@reviewjournal.com or 702-383-0336. Follow @MaryHynes1 on Twitter. Review-Journal staff writers Michael Scott Davidson and Bill Dentzer contributed to this report.