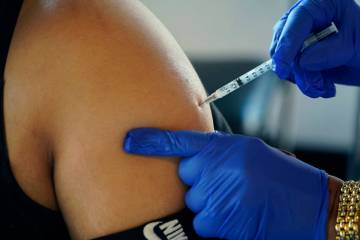
Home care aides balance personal safety with sense of duty
After learning that an elderly client had developed symptoms similar to those of COVID-19 in mid-March, personal care aide Kismet Evans immediately called her employer and self-quarantined.
After a month off without pay, Evans returned to work. Her employer, A Caring Hand, provided her with two packs of gloves, a few surgical masks and a small bottle of hand sanitizer, she said.
Returning to work was not an easy decision, said Evans, 58, adding that the rudimentary supplies did not make her feel she could safely do her job.
“We are fatigued and afraid,” she said of herself and colleagues who work for other home health care companies in the Las Vegas Valley.
It’s a dilemma faced by many of the roughly 11,550 home health and personal care aides in the Las Vegas area, a figure that does not include some nurses who work in hospice care or perform other medical tasks for housebound patients.
Many so-called PCAs earn just a few dollars over minimum wage and are expected to supply their own protective gear and cleaning supplies so they can safely visit clients in their homes.
“It’s ridiculous,” Evans said, referring to her employer’s practice of distributing one package of PPE to its workers. “Do I take the money out of my pocket to buy hand sanitizer or do I buy food and pay a bill?”
A Caring Hand manager Fernando Jimenez said the company has tried to provide PPE for its workers but only recently was able to obtain face masks for personal care aides.
The agency is also limited to buying one case of 56 small bottles of hand sanitizer at a time for $160. Asked if he thinks there should be legislative action to help agencies obtain PPE equipment, Jimenez said: “To me that would be the best thing to do to make sure we’re keeping our workers safe.”
Despite their low compensation, personal care aides provide a crucial lifeline to their housebound clients, many of them elderly or disabled. In addition to duties like grocery shopping and providing companionship, they help clients with essential daily activities like bathing, eating and cooking.
‘I felt it was my responsibility’
It is work that makes it impossible for them to keep their distance from clients and family members who live with them.
Evans, a California native who moved to Las Vegas several years ago to take care of her elderly parents — both of whom have health issues — said the trade-offs that come with the job have been crystallized by the coronavirus pandemic.
“I have to be cautious because I wouldn’t want to get my parents sick because — God forbid — I don’t think my mom would survive it,” she said.
But in addition to needing the income to help her parents with housing, food and medication, Evans said she felt an obligation to her 62-year-old client, who recovered from her illness but was never tested for COVID-19.
“After speaking to my patient after 30 days and hearing how lost … (she) was without me and how she struggled to try and maintain without me — it was heartbreaking to hear,” Evans said. “I felt it was my responsibility.”
The Review-Journal spoke with four other PCAs, all of whom spoke on condition of anonymity because they said they feared retaliation from their employers.
Three of the four, who work for different agencies in the valley, said they also have to pay for their own gloves or face masks and don’t feel safe because they are frequently unable to find the equipment, which remains in high demand.
Evans said she gets up early to try to find the supplies she needs.
“I’m at the stores at 5 or 6 a.m. in the line just so I can get supplies so I can protect myself to get to work,” she said.
PCAs are right to worry about their health, since many are part-time workers and do not receive health care or sick leave through their employers, said Brian Shepard, chief of staff of the Nevada chapter of Service Employees International Union (SEIU), Local 1107.
Of the personal care aides the Review-Journal spoke to, only one received health insurance through their employers.
Paid sick leave a question mark
Though they work with a population that is most at risk of developing serious complications if they contract COVID-19, the aides all also said they had not been given clear direction on whether they would be paid if they had to self-quarantine after being exposed to the disease. Nor were they told what they should do if a client was exposed to the coronavirus, they said.
Jimenez, manager for A Caring Hand, said the agency has a clear policy on dealing with COVID-19.
When one patient was diagnosed with COVID-19, the caregiver was immediately placed on quarantine, he said. That employee is still under quarantine, though Jimenez did not say if the worker had tested positive.
If an employee believes they have been exposed to the coronavirus on the job, the agency refers them to UNLV to get tested. Employees who test positive get paid leave, according to Jimenez. If an aide feels uncomfortable going to a home, he or she is able to leave, he added.
The median hourly wage for personal care aides is $11.47 with an annual median wage of $23,850. Typically, a high school diploma or equivalent is required for entry-level jobs, although employees also complete formal training and tests through their agencies, according to a May 2019 report from the U.S. Bureau of Labor Statistics.
Shepard, the union official, said that creates a situation where both worker and client are endangered.
“These are underpaid workers — that’s a huge public health risk,” he said.
SEIU is organizing home care workers in an effort to change the home care system. The plan is not to bargain with individual employers, but to push for legislative action to address the issue, according to Shepard.
To call attention to the issue, Local 1107 sent a petition demanding more protections for home care workers, including access to PPE, training, screening and testing and mandated sick leave, and their clients to Gov. Steve Sisolak’s office last month.
“There is the way the system is structured right now, which is rigged against home care workers. Historically, they have been written out of laws that provide basic workplace protections,” Shepard said. “We are organizing people to call for improving standards by advocating for a sustainable long-term care system. That is going to require legislative action, that’s how home care workers will win livable wages and basic benefits.”
Evans, who agrees that legislative fixes are needed, said clients will suffer if the industry’s long-standing problems are not addressed.
“We’re their extended family, advocating for them with SNAP and doctors,” she said. “We don’t want to leave them.”
Contact Alex Chhith at achhith@reviewjournal.com or 702-383-0290. Follow @alexchhith on Twitter.
Challenges amid pandemic
While thousands of businesses in Nevada remain closed because of an order from Gov. Steve Sisolak, business has been robust at local health care agencies, seven of which were hiring in the Las Vegas area as of last week.
The BrightStar Care branch in central Las Vegas is among them, but not because it has had a problem with workers leaving, owner Becky Torrez said. When some employees chose not to work because of underlying health conditions, she said, staff started calling former workers to see if they would be interested in coming back to work during the pandemic.
"We have an awesomely loyal staff," Torrez said, adding that most employees have continued to work. "We've done a good job of maintaining our bench of people." (None of the personal care aides interviewed for this article worked for BrightStar.)
Torrez said the agency provides PPE to its personal care aides and goes to great lengths to ensure it doesn't run out.
"We get on Amazon early in the morning and late at night," Torrez said, adding that the agency orders just enough equipment to meet its needs so other health care workers aren't shut out.
Torrez commended the work of her employees and other personal care aides across the valley. The work that aides do isn't just important during the coronavirus pandemic, she noted.
"It's a noble thing to do," Torrez said. "They are helping to keep our elderly safe."