Got Medicare? Get a no-cost COVID-19 test
If you have Medicare and want to be tested for COVID-19, I have good news.
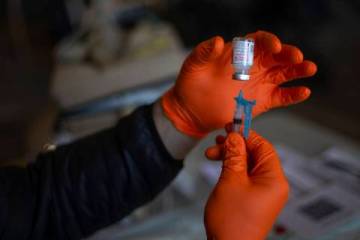
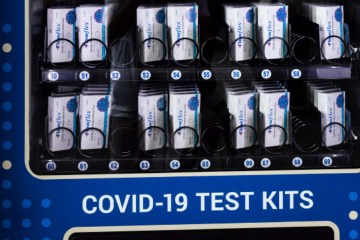
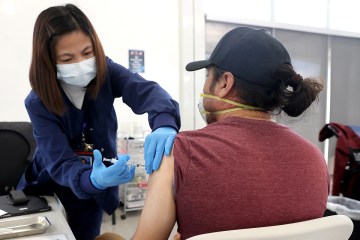
Medicare covers tests with no out-of-pocket costs. Beneficiaries can get tested at home, a doctor’s office, a local pharmacy or hospital, a nursing home or a drive-up site. Medicare does not require a doctor’s order for testing.
Testing is particularly important for older people and nursing home residents, who are often among the most vulnerable to COVID-19. Widespread access to testing is a crucial precursor to a safe, gradual reopening of America.
When a vaccine for COVID-19 is developed, Medicare will cover that, too.
For Medicare beneficiaries who are homebound and can’t travel, Medicare will pay for a trained laboratory technician to come to your home or residential nursing home to collect a test sample. (This doesn’t apply to people in a skilled nursing facility on a short-term stay under Medicare Part A, as the costs for this test, including sample collection, are covered as part of the stay.)
If you receive Medicare home health services, your visiting nurse can collect a sample. Nurses working for rural health clinics and federally qualified health clinics also can collect samples in beneficiaries’ homes under certain conditions.
Or you can go to a parking lot test site set up by a pharmacy, hospital or other entity in your community.
We’re doing similar things in the Medicaid program, giving states flexibility to cover parking lot tests as well as tests in beneficiaries’ homes and other community settings.
We also implemented the Families First Medicaid eligibility option, which allows states to cover tests for uninsured people with no cost-sharing. Individuals should contact their state Medicaid agency to apply for this coverage.
Medicare and Medicaid cover serology or antibody tests for COVID-19. These tests can help identify who has been exposed to the virus.
Medicare generally covers the entire cost of COVID-19 testing for beneficiaries with Original Medicare. If you’re enrolled in a Medicare Advantage health plan, your plan generally can’t charge you cost-sharing (including deductibles, copayments and coinsurance) for COVID-19 tests and the administration of such tests.
In addition, Medicare Advantage plans may not impose prior authorization or other utilization management requirements on the COVID-19 test or specified COVID-19 testing-related services for the duration of the public health emergency.
We have also required that private health issuers and employer group health plans cover COVID-19 testing, and certain related items and services, with no cost-sharing during the pandemic. This includes items and services that result in an order for, or administration of, a COVID-19 diagnostic test in a variety of medical settings, including urgent care visits, emergency room visits and in-person or telehealth visits to the doctor’s office.
From day one, Medicare has worked to ensure that cost is no barrier to being tested for COVID-19, and to make testing as widely and easily available as possible. As a result, we’ve seen a surge in testing among Medicare beneficiaries.
Contact Medicare at 800-MEDICARE (800-633-4227).
Seema Verma is administrator of the U.S. Centers for Medicare & Medicaid Services.