COVID-19 testing meant separation for young Las Vegas family
First came the cough.
It was unlike anything his parents had heard before. Deep, dry and desperate, like a plea for help.
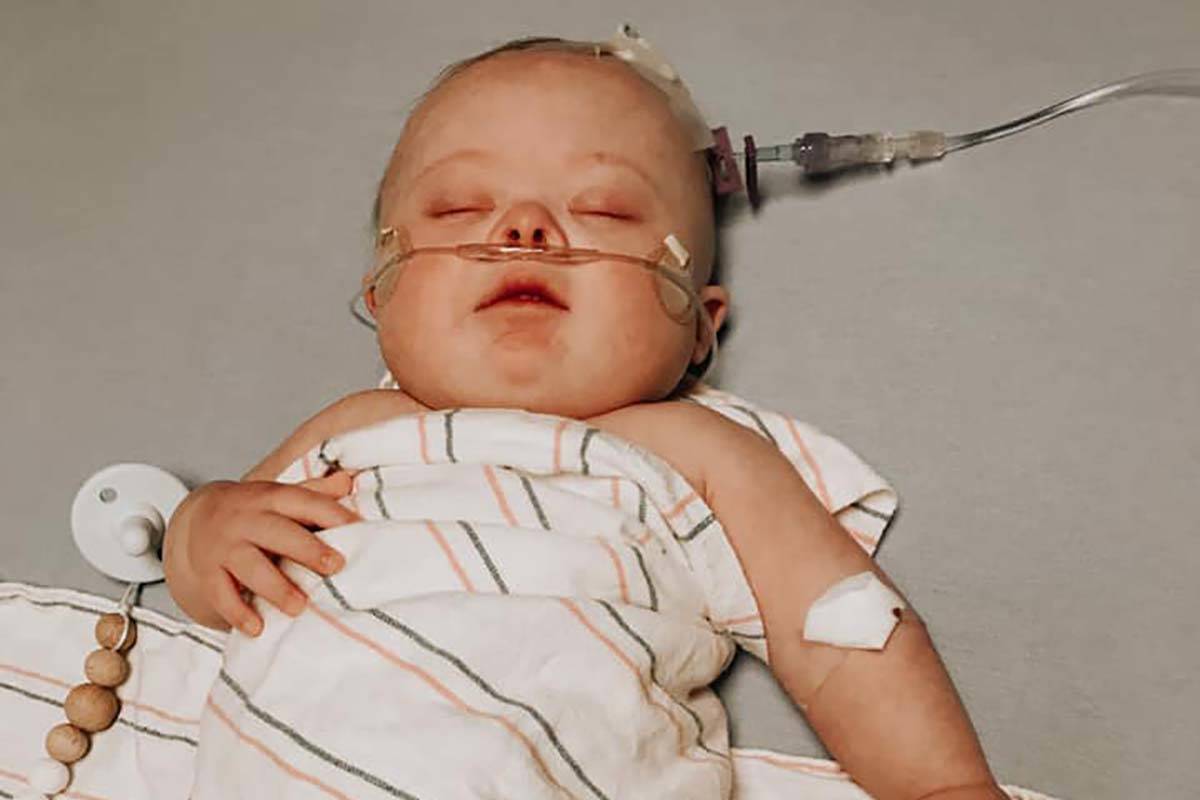
Within 48 hours, 9-month-old Caleb Anderson would be quarantined at Summerlin Hospital Medical Center, his condition rapidly deteriorating as doctors tested him for the novel coronavirus.
Because of his symptoms, hospital staff had no choice but to separate the Anderson family, a divide that came on as abruptly as the symptoms that took over Caleb’s little body.
But on Thursday afternoon, days earlier than expected, Caleb’s test results came back: They were negative for COVID-19 but positive for hMPV, or human metapneumovirus, a respiratory infection with symptoms identical to the new coronavirus.
Rachael and Cody Anderson let out a sigh of relief. God had answered their prayers, and their son’s negative test results ended what could have been a minimum two-week separation.
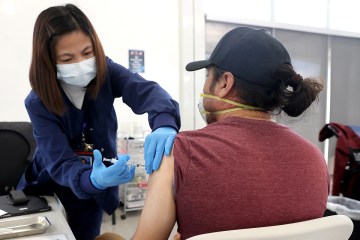
Even so, the Anderson family’s experience offers an intimate glimpse into the lonely and isolating process of coronavirus testing, and how some doctors in the Las Vegas Valley are proactively treating patients who show symptoms of COVID-19 while waiting for confirmation.
“I can only compare the process of being tested to the story in the Bible of leprosy,” Rachael Anderson, who had been quarantined with her son, said Thursday. “No one can come close to you, no one wants to come close to you, and no one wants to talk to you. It makes you feel so isolated.”
An extra chromosome
To date, according to the Centers for Disease Control and Prevention, adults make up most known cases of the coronavirus, which is said to cause severe illness in those 65 and older or in individuals with underlying medical conditions.
If Caleb had tested positive for COVID-19, he would have been among the less than 0.3 percent of patients in Southern Nevada younger than 4.
But to his doctors and parents, such an unlikely test result seemed possible because of Caleb’s complicated medical history.
At 13 weeks, an ultrasound revealed that Caleb had an extra chromosome. At 29 weeks, doctors noticed he had stopped growing inside the womb.
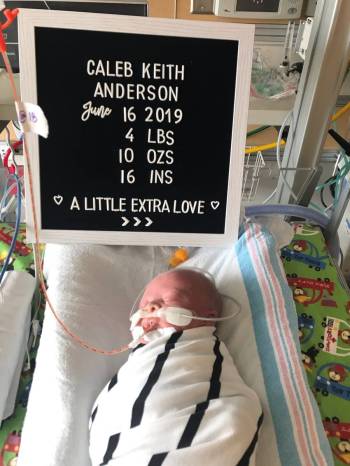
Caleb arrived just over a month later, at 34 weeks, on a hot day in June after an emergency cesarean section. He was barely alive.
Later that day, the Andersons met their son for the first time. He was swaddled in a black-and-white striped blanket and hooked up to tubes and machines in the neonatal intensive care unit.
The machines rumbled and beeped, but Caleb slept peacefully. He was so tiny, weighing just 4 pounds, 10 ounces. His small head was fuzzy like a peach.
He was perfect.
“I had so much fear after the Down syndrome diagnosis, but when I met him, I knew in that moment I’d never want to change him for the world,” Rachael Anderson said.
Caleb spent the next two months in the NICU before finally going home with his parents. He suffers from a congenital heart defect, a compromised immune system and a chronic lung disease common in premature babies.
Since leaving the NICU that first time, Caleb has been admitted to the hospital more than 10 times with different viruses, according to his mother. This go-round, Caleb’s doctors thought he might have been exposed to COVID-19 in early March, during his last hospital stay after he came down with the flu.
Precautionary treatment plan
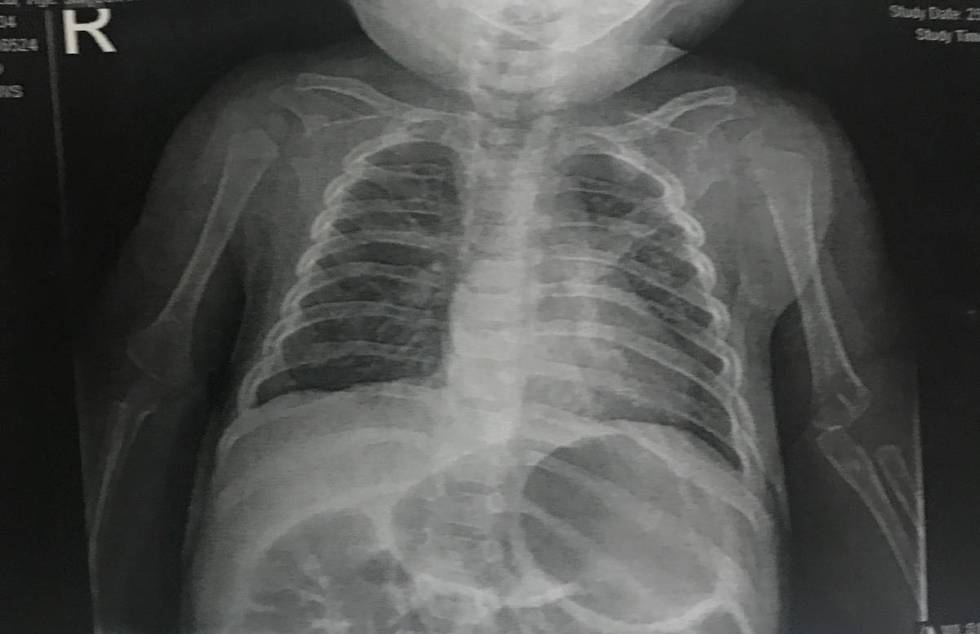
By the time Caleb arrived at the hospital around 3 a.m. Wednesday, his oxygen level had plummeted and his temperature had spiked to 104.5 degrees.
Familiar with Caleb’s medical history, his doctors immediately took him in for a chest X-ray, and soon, the black-and-white image showed that the boy’s airway had collapsed.
Around the same time Caleb was admitted, his father, who had parked the car while his wife ran inside, was being turned away at the doors of the hospital.
“It was kind of a luck of the draw,” Cody Anderson said. “Rachael brought him in, so Rachael got to stay.”
Even before the chest X-ray, doctors suspected Caleb had contracted the coronavirus and committed to a proactive treatment plan as though the boy’s test already had come back positive.
The 23-year-0ld father turned around, got back in his car and drove home alone.
As a precaution, Caleb’s doctors also had asked Cody Anderson to self-quarantine. Separated from his family, he sat at home for nearly two days, anxiously awaiting updates from his wife.
Temporary but mandatory separation
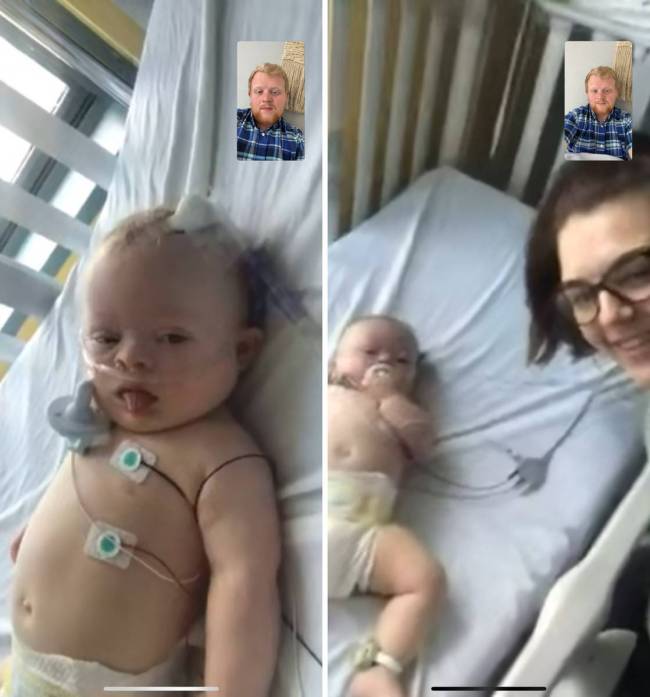
While apart, the Andersons could interact only through their phone screens — a situation all too common amid a global pandemic that has essentially shut down the entire country and forced people to work and study from home.
Coast to coast, including here in Nevada, doctors and nurses have struggled with the unfathomable reality that their patients are dying alone.
As of Thursday morning, Caleb’s condition had stabilized and his fever had gone down, though the boy still was “coughing like crazy” and struggling to breathe, his mother said.
Doctors have him on high-flow oxygen support, a form of respiratory therapy, and different medications.
Though the Andersons received the result they prayed for this time, Caleb’s mother suspects there will be many more scares. Between Caleb’s frequent doctor visits and hospitalizations, the boy generally has a higher risk of exposure than the average infant, his parents said.
“I know it’s hard staying at home for days on end, but you have to think about what’s best for everybody,” Caleb’s father said, pleading with the public to take social distancing guidelines seriously. “Especially for those who can’t take care of themselves or are immunocompromised, like my son.”
Contact Rio Lacanlale at rlacanlale@reviewjournal.com or 702-383-0381. Follow @riolacanlale on Twitter.