While COVID-19 picture improves, Nevada’s rural hospitals still challenged
Hospitals in rural Nevada still face shortages of beds, staff and supplies as they bear the brunt of the delta surge that has waned elsewhere in the state, officials said Thursday.
Even with the delta surge receding across the state, “Rural hospitalizations remain near their peak,” said Talus Analytics’ Ellie Graeden, a consultant to the Nevada Department of Health and Human Services.
Intensive care units and COVID-19 wards remain full, said Joan Hall, president and CEO of Nevada Rural Hospital Partners, an alliance of 13 small rural hospitals. However, fewer patients now than in July or August need to be transferred to hospitals elsewhere in the state for higher levels of care.
Graeden and Hall spoke during a bi-weekly news briefing on COVID-19 by state officials.
“Staffing is also a true challenge, as it is across the state and nationwide,” Hall said. Potentially heightening the challenge is a federal vaccination requirement for workers in most health care settings that receive Medicare or Medicaid reimbursement.
“That has been a huge concern for rural hospitals,” Hall said, noting that staff vaccination rates vary from 60 percent to 90 percent at Nevada’s rural hospitals.
“We know that there are staff members who will refuse to be vaccinated,” she said. “And we don’t know yet if President Biden’s regulation is going to provide for testing in lieu of vaccinations.”
Although staffing is an issue at hospitals in both urban and rural settings, “Losing one nurse or one social worker or one provider in a rural community is a huge strain on the system,” she said.
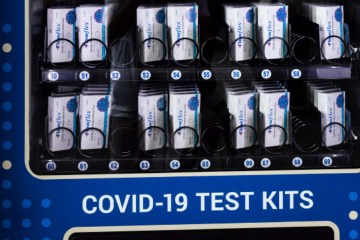
Due to supply-chain issues, the rural hospitals are struggling to obtain supplies such as test kits and oxygen cylinders for patients ready to be discharged, Hall said.
One state strategy for easing the burden on rural hospitals is to increase the availability of monoclonal antibody treatment, a one-time IV infusion designed to keep people who have tested positive for COVID-19 out of the hospital.
The state Board of Examiners this week approved a federally funded $30 million contract for mobile outpatient monoclonal antibody treatment.
“These treatments will help in areas of high caseload and low vaccination rates, including our rural communities,” DuAne Young, policy director for Gov. Steve Sisolak, said at Thursday’s briefing.
In Elko County, for example, more than 60 people have received the therapy at a clinic at Great Basin College since Oct. 1, he said.
Monoclonal antibody treatments reduce the risk of hospitalization by 70 percent when given within 10 days of the onset of symptoms, Dr. Michael Anderson, a senior adviser to the U.S. Department of Health and Human Services, said at a briefing in August.
There no longer are strict requirements for who can receive the treatment, beyond being over the age of 12 and more than 88 pounds, if a doctor believes the patient is at heightened risk for serious disease.
Lower vaccination rates in some rural areas are contributing to the strain on hospitals, Hall said.
“Certainly, that does increase the number of patients that we’re seeing in our ERs or that are being admitted, and causes staff great concern,” she said.
“I think there’s a lot of fatigue in nurses and providers seeing patients that they know,” she continued. “In rural areas, everyone knows everyone. And when you see that grandma and grandpa, or your next door neighbors, who are unvaccinated coming in with COVID symptoms and are very sick, it causes great strain.”
Contact Mary Hynes at mhynes @reviewjournal.com or 702-383-0336. Follow @MaryHynes1 on Twitter.