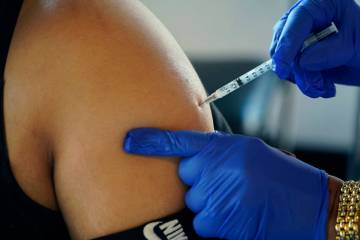
Routine medicine goes on despite coronavirus pandemic
Dr. Staci McHale’s baby-delivering garb is a barometer of how routine medical care has changed in the age of the new coronavirus.
Usually McHale wears a surgical mask, gloves and other basic protective gear when delivering babies. These days, that standard array has been augmented by an N95 mask covered with a surgical mask that, McHale said, makes it difficult enough to talk through, much less guide a patient through a delivery.
“It’s something I never thought I’d have to be in,” McHale said. “I haven’t put on makeup below my eyes in almost a month.”
The outbreak also has introduced McHale, an obstetrician-gynecologist, to other things she never imagined would be part of her medical practice. “I never thought I’d be teaching my patients how to properly wash their hands and how important it is to wear a face mask in public.
“It’s all a little surreal,” she said. “Almost like living on another planet.”
Surreal is as good a word as any to describe how, even in the midst of a global pandemic, routine medical care — preventive checkups, pediatric visits, births, even the occasional trauma surgery — continues in a way that’s surprising to both doctors and patients.
Strange times
“We are practicing medicine in an environment none of us ever could have predicted,” said Dr. Daniel Burkhead, an anesthesiology and pain management physician, who is president of the Clark County Medical Society.
“It seems as though every day I wake up and the numbers are changing, and implementation of how we are going to continue to provide care for our patients is changing.”
Patients, too, have awakened to a new, unwelcome medical reality. Some, Burkhead says, are putting off trips to doctors for routine checkups, even for “problems of a more urgent nature, trying to deal with problems rather than going to a health care environment.”
Even doctors have reservations now. Dr. Mitchell Forman, a rheumatologist, said that “after practicing almost 50 years, this is the first time in my life that I’m apprehensive regarding my health when I go to work, and for my family as well.”
“I’m also very much concerned about my patients,” added Forman, some of whom take immunosuppressive medications that can increase their risk of contracting COVID-19.
Carrying on
In just about every medical specialty, however, “there are issues that aren’t going away,” Forman said. “So you have diabetes, you have high blood pressure, you have mental issues and heart disease. So the focus can’t just be on COVID-19. It’s an important determinant, but it can’t be only on that. You have to think of other health issues patients have.”
Dr. Pamela Greenspon, a pediatrician, still is seeing young patients for shots and wellness checkups — although she now reserves morning appointments for children who aren’t ill.
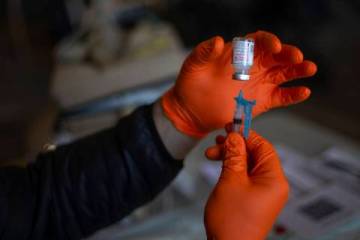
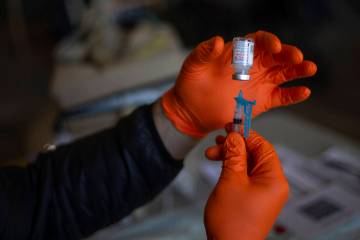
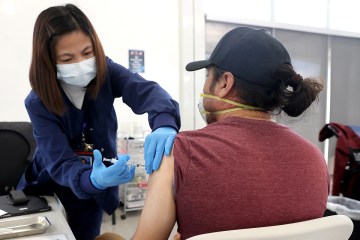
“We especially want to make sure that children who need vaccinations receive vaccines,” she said. “We don’t want to see a measles surge or an increase in whooping cough.”
McHale continues to see expectant mothers, and the coronavirus is an unpopular but necessary topic of discussion during office visits.
“There are times that we are the first faces our patients have seen for the last three or four weeks,” she said. “They have been social distancing. They’re terrified, and staying at home, as they should.”
But even with a pandemic hovering in the background, “it’s our job to keep this a happy event, to make sure when they have a delivery that they (have) the outcomes they deserve and to make sure they stay safe,” McHale said.
Dr. George Alexander, a plastic surgeon, hasn’t performed an operation in weeks. His practice consists mostly of elective procedures. The day after Gov. Steve Sisolak’s address announcing a halt to elective procedures, “I canceled all of my surgeries and I haven’t performed one since.”
The goal is to reserve vital protective equipment and resources for first responders and to ensure safety for both patients and health care professionals. Alexander supports the move. But, he said, “it’s made a huge impact on doctors and patients.”
Logistics
Even while continuing to provide necessary care, doctors have modified their ways of doing business. Patients who see Alexander for follow-up appointments are asked to call the office receptionist when they arrive and are escorted inside. Patients also are screened for COVID-19 symptoms before entering, and drivers and other family members are asked to wait outside.
Greenspon’s office is spacing appointments further apart to prevent crowded waiting rooms, and most area medical practices have adopted telemedicine — examining patients via videoconferencing — when an office visit can be safely postponed.
Dr. Thomas Hunt, a family practice physician, estimates that 90 percent of his practice now consists of videoconferencing, although it’s not appropriate for every complaint or every patient.
“We still keep slots open for people who need to come in to have procedures or need to be seen in person,” Hunt said.
Equipment
The pandemic also has focused attention on some aspects of medical practice that were previously taken for granted. Dr. Deborah Kuhls, a trauma and general surgeon, said she and her colleagues have become “very mindful of how many people go into” protective gear when treating a patient who arrives from a shooting, car accident or other trauma.
“We didn’t used to think about how many people we had gowned and masked,” she said. “We always used universal precautions, but (now) we try to conserve while still ensuring our patients are safe.
“We don’t want to overuse something so that other health care professionals would have less.”
Contact John Przybys at jprzybys@reviewjournal.com or 702-383-0280. Follow @JJPrzybys on Twitter.