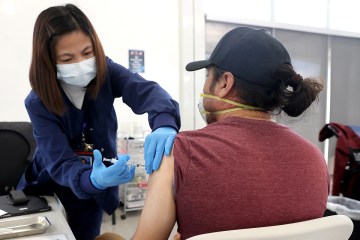
Nevada hospitals move closer to capacity, postpone surgeries
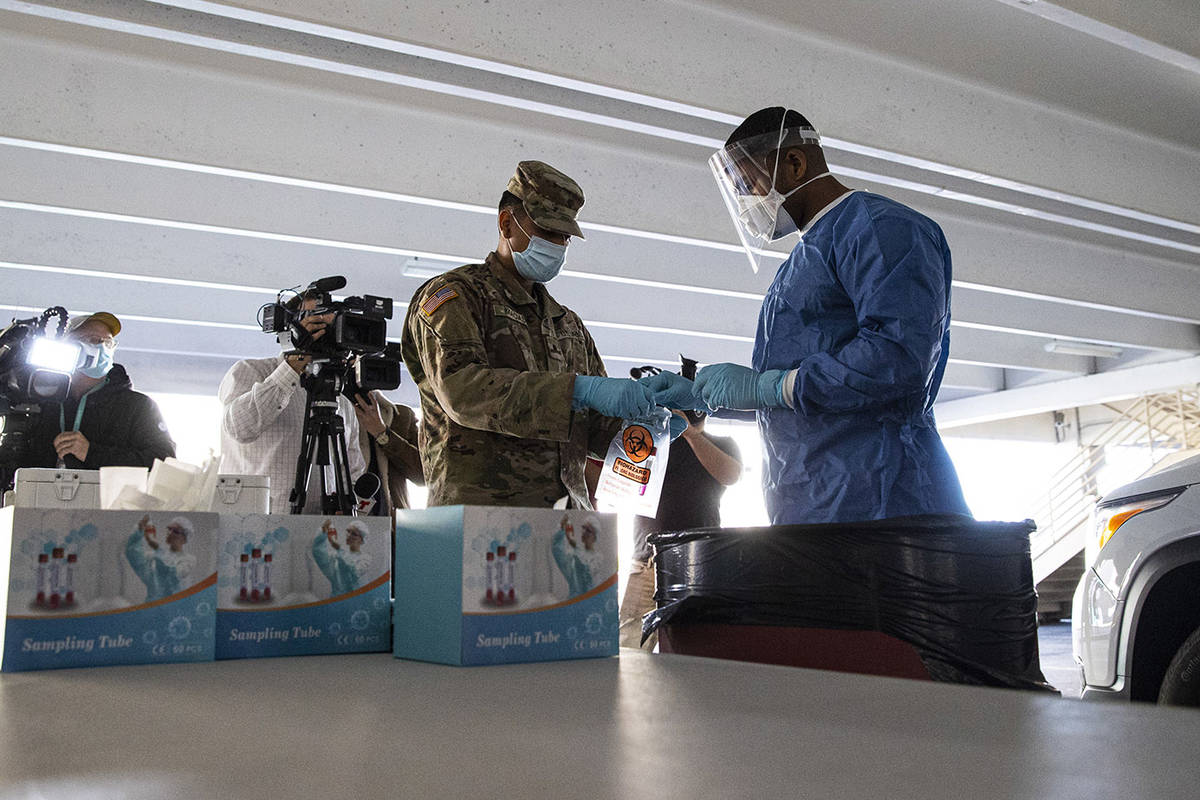
Southern Nevada hospitals moved closer to capacity on Monday, with some postponing elective surgeries and taking other measures to meet the growing wave of COVID-19 patients.
Eighty-seven percent of licensed hospital beds were filled in Southern Nevada, and 82 percent statewide, according to the Nevada Hospital Association. COVID-19 cases made up nearly one-third of all hospitalized patients in the state and more than one-third of patients in intensive care units.
At University Medical Center in Las Vegas, staff members are working an extra day a week, and administrators have shifted to caring for patients to handle the escalating surge, said hospital CEO Mason Van Houweling.
“Over the weekend, it was all hands on deck for our teams to care for patients,” he said.
As a result, elective surgeries scheduled for this week at UMC are being delayed, he said, and post-surgery recovery areas are being converted into intensive care unit space.
As of Monday, the number of hospitalized COVID-19 patients statewide had more than doubled— from 692 to 1,617 — since a month ago, the hospital association said.
Across rural Nevada, 95 percent of ICU beds were filled, with Churchill, Elko, and Humboldt counties along with Carson City being at or beyond capacity.
‘Biggest wave we’ve had’
The demand for mechanical ventilation equipment, used to assist patients with breathing, increased in excess of 250 percent, with these cases rising to 227 from 89 in the past month.
“This is far and away the biggest wave we’ve had since we had our first patient come into the valley in the beginning of March,” said Dr. Joe Corcoran, the chief medical officer overseeing HCA Healthcare hospitals in Nevada and California, including the four Sunrise Health System hospitals in Las Vegas.
Las Vegas is seeing some of the highest volumes of COVID-19 across the company’s network of 185 hospitals in nearly half the states, Corcoran said. From its other hospitals, the company is bringing in some of the equipment and medications needed to treat patients here.
“The one thing that we can’t bring in is additional staffing” from other HCA hospitals because of the intense demand across the country, he said.
“My profound respect is owed to our amazing people who keep showing up doing incredible work under very difficult circumstances,” he said.
The Sunrise hospitals are curtailing elective surgeries but not eliminating them.
“Some of those cases that were elective in March are not so elective any longer,” he noted. “We have started to reel in procedures, particularly … those that would be reasonably expected to tap into beds, ICU space, ventilators, level of care, that really should be prioritized for patients with COVID.”
The three St. Rose Dominican hospitals in the valley currently are not postponing elective surgeries.
“Delaying such procedures can negatively impact the health of our patients,” spokesman Gordon Absher said in an email. “We have gone to great lengths to secure additional staff, including traveling nurses, to care for any surge in patients.”
The Valley Health System, with six hospitals in the valley, is employing other strategies to free up hospital beds, including working closely with skilled nursing homes and other facilities for timely discharge of patients, spokeswoman Gretchen Papez said in an email.
Hospital representatives note that since the start of the pandemic, hospital treatments for COVID-19 have improved, intensive care is required less frequently, and the length of stays has decreased.
Thanksgiving effect
Public health officials had predicted that cases of the coronavirus could intensify the surge in the aftermath of Thanksgiving if people ignored warnings to avoid travel and large gatherings.
State officials said on a press call Monday that it was still too soon to feel the full effect of the holiday. The incubation period for the virus is 14 days, meaning that some people will not fall ill until two weeks after exposure.
“Our expectation is that the surge we’re experiencing prior to Thanksgiving will continue and that we need to be prepared for increased hospitalizations on the other side of that,” said Caleb Cage, director of the state’s COVID-19 response.
Tracking the spread of COVID-19 in Nevada through data
The state on Monday reported 2,448 new cases of COVID-19 and four additional deaths, bringing the cumulative case count in the state to 170,587 and total fatalities to 2,319.
The daily average of new cases over the past week jumped to 2,631, a new high. The daily average for deaths in the week was down slightly, dropping to 25 from 26.
The positivity rate, measured by the Review-Journal as the number of people who test positive out of total tests, increased to a record 16.59, up slightly from 16.46 on Sunday. The rate has been rising steadily since mid-September.
The state, which calculates the rate differently, reported a rate of 21.2 percent over the past 14 days.
“Will it get much worse or is it starting to flatten out?” Corcoran said about the surge. “We’re actually seeing some projections that suggest that the rate of rise will start to level off.
“But there’s no doubt we’re in for a bumpy couple of weeks.”
Contact Mary Hynes at mhynes@reviewjournal.com or 702-383-0336. Follow @MaryHynes1 on Twitter. Review-Journal staff writer Michael Scott Davidson contributed to this report.