Henderson man’s COVID-19 battle highlights risk of high blood pressure
Mark StHilaire knew he had high blood pressure when he was diagnosed with COVID-19, but he didn’t realize that the underlying health condition put him at risk of serious complications from the disease.
The 46-year-old Henderson resident quickly discovered how serious the combination of hypertension — the medical term for high blood pressure — and the illness caused by the new coronavirus can be after his symptoms first appeared on March 12.
“I’m not a smoker. I had high blood pressure and was on medication for a year for it,” he said. “It came on so fast, once that cough started, it progressed (and) after a few days and my lungs were filled with fluid.”
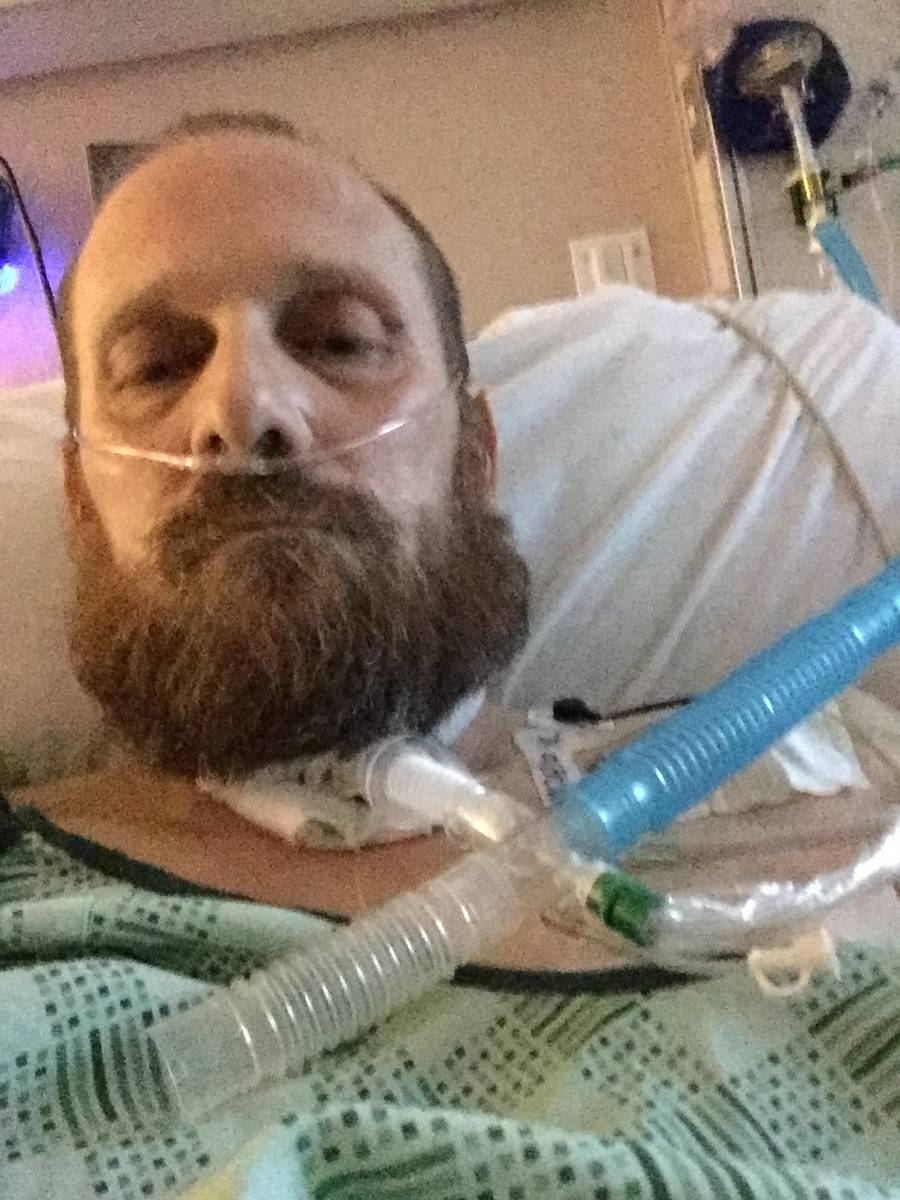
He ultimately spent 47 days in the hospital, 31 of which he was sedated and intubated. He suffered kidney failure, sepsis, memory loss and now has a hole in his throat from a tracheostomy doctors had to perform before being discharged in early May.
But during his recovery at home, StHilaire started feeling chest pain. When he returned to the hospital, doctors found blood clots – an increasingly common side effect of COVID-19. He was finally discharged for the second time on May 21.
StHilaire suspects he contracted the disease through his job on the Strip or flights to and from a wedding in Georgia.
After being admitted to Centennial Hills Hospital, he was quickly sedated and intubated, a common practice in serious cases of COVID-19. He ended up being unconscious for the remainder of his days there. After he tested negative for the coronavirus, StHilaire was transferred to PAM Specialty Hospital where he awoke to continue his recovery.
‘I wasn’t the same person’
“When I woke up, I remember looking down at my arms and legs and face, in the mirror,” he said. “I wasn’t the same person.”
StHilaire, who lost 60 pounds during the ordeal, believes his family suffered more than he did. His wife and five children were unable to see him during his stay in the hospitals and recorded messages for him on a CD. Nurses told the family that StHilaire had tears coursing down his face as he listened to them.
“It was harder on them than me. I was sleeping the whole time,” he said of his family. “They didn’t know if dad was going to come home. They couldn’t call and see me.”
StHilaire’s complications are not uncommon in COVID-19 patients.
Across the nation, approximately 46 percent of adults in the United States have high blood pressure, according to the American Heart Association.
Though scientists are still studying what makes certain demographic groups more susceptible to the coronavirus, preliminary evidence suggests high blood pressure is a major risk factor, said Dr. Alona Angosta, associate professor at UNLV School of Nursing.
When researchers studied 5,700 hospitalized coronavirus patients in the New York City area, 56.6 percent had high blood pressure, 41.7 percent were obese and 33.8 percent had diabetes, according to a peer-reviewed study published in the Journal of the American Medical Association in April.
Top risk factor in Clark County
The results of that study are similar to data on the outbreak in Clark County, with the Southern Nevada Health District listing high blood pressure as the top underlying health issue among people who have been hospitalized and died. Diabetes is the second on the district’s list, which does not include obesity data.
While the evidence that high blood pressure is a significant risk factor for those infected by the new coronavirus is growing, it’s not clear why the risk is increased.
“There is lack of sound evidence why individuals with (hypertension) are susceptible to COVID-19 and have more complications than those without high blood pressure,” Angosta said, adding that the general weakening of the immune system that occurs in patients with high blood pressure may play a role.
But some experts theorize that certain hypertension medications that stimulate specific receptors in the lungs, where the coronavirus attaches itself in the course of infection, could adversely affect how a person combats the virus.
The heart association, however, advises people to continue to take their medication as prescribed, since there is no direct evidence linking such drugs to increased risk from the virus.
More will be learned as scientists continue to study the coronavirus, Angosta said.
“Scientists are looking into why this is so,” she said. “Then we can advise patients with high blood pressure to be more vigilant and cautious because of their weakened immune systems.”
An inspiring recovery
StHilaire was one of the most inspirational and uplifting patients that have come out of the PAM hospital since the pandemic started, said his father-in-law Wayne Tunheim, 61, who works there as a registered nurse.
Tunheim was able to watch StHilaire recover from memory loss and relearn how to walk.
When StHilaire correctly responded to neurologists, shortly after he woke up, they gave each other a high-five, Tunheim recalled. When he took his first steps down the hall, nurses and doctors cheered for him.
It marked a change in tone for the hospital, which saw a stream of COVID-19 patients admitted, causing a shortage of personal protective equipment.
“He motivated a tremendous amount of people. We see a lot of people get sick, and it’s great to see someone get better,” Tunheim said.
Contact Alex Chhith at achhith@reviewjournal.com or 702-383-0290. Follow @alexchhith on Twitter.