Coronavirus advice for Las Vegas: Prepare for worst, but don’t panic
Dr. Judith Ford reflected on a top U.S. health official’s warning this week that the new coronavirus ultimately would spread in communities in this country.
The message was “you need to be prepared,” Ford, medical director of clinical quality for HealthCare Partners Nevada, recounted Wednesday.
“But what does that mean?” she asked. “I think it was kind of a scary announcement.”
Ford and other Southern Nevada health authorities interviewed Wednesday stressed there is no need to panic, noting that the risk in the U.S. of contracting COVID-19, the respiratory illness caused by the coronavirus that emerged out of China, remains low. And plans already in place for addressing public health emergencies are being refined to respond to the threat.
“It’s important to prepare for the worst,” said Dr. Vit Kraushaar, medical investigator for the Southern Nevada Health District. “We can always hope that the worst doesn’t happen, but better to be safe than sorry.”
A 2017 federal plan for addressing a flu pandemic, such as the swine flu of 2009, is serving as a guide for preparing for the possibility of a COVID-19 outbreak in the U.S. There have been 60 cases in this country, including 42 people who returned to the U.S. after they became infected aboard the Diamond Princess cruise ship.
There have been no known cases in Nevada.
‘Groundwork’ laid
“Even though this is a new disease and can seem intimidating, thankfully, much of the groundwork has been laid by past pandemic flu planning,” Kraushaar said.
The 2017 document by the Centers for Disease Control and Prevention provides for an escalating response to a pandemic — a worldwide spread of a new disease — depending on its severity.
For example, the plan shows that “cancellation of school for certain amounts of time was effective for stopping the spread of influenza,” Kraushaar said. A less extreme measure in schools would be for children to be kept in smaller groups or for desks to be spaced farther apart.
To answer questions about the coronavirus, the health district is planning a face-to-face briefing with Southern Nevada emergency response officials, including municipalities and hospitals, a district spokeswoman said.
Nevada hospitals said they’ve been coordinating with public health authorities to respond to the threat.
The Nevada Hospital Association said in a statement that it has been “in constant contact with our county, state and federal public health officials and has been monitoring the disease spread and briefing hospital infection disease and preparedness personnel since early January.”
Las Vegas’ public hospital, University Medical Center, said it also has been gearing up.
“For the last several weeks, we have been working closely alongside the Southern Nevada Health District and the U.S. Centers for Disease Control and Prevention to develop protocols for screening, testing and managing patients who might present with COVID-19 infection,” Dr. Shadaba Asad, UMC’s medical director of infectious disease, said in a statement.
“With cases of coronavirus increasing across the world, we recognize that community members have concerns and fears. At UMC, we believe that the antidote to this fear is knowledge and preparedness,” she said. “We feel confident that UMC is fully prepared to deal with this infection, if and when it affects our community.”
The CDC has made recommendations to hospitals and practitioners on how to conserve resources such as masks and gloves that are in high demand during an outbreak of contagious illness.
“Currently, only a small percentage of Nevada hospitals have indicated that PPE (personal protective equipment) is in short supply, while many are indicating that they are seeing items on back order,” the hospital association said.
“The health care sector has seen preemptive strategies put in place to help secure this critical supply chain,” the association said.
What individuals can do
Though consumers have been stripping store shelves of face masks since January, health authorities aren’t recommending masks for the general public, except for individuals who are ill to prevent their coughing and sneezing from infecting others.
The type of preparedness that the CDC and other health authorities currently recommend revolves around thinking through certain scenarios.
“If you had small children, you need to think, ‘What would happen if our day care shut down?’ ” said Ford. “If you had an office job, ‘Would I be able to work from home?’ Also, ‘How do I reach my health care provider if I get sick?’ ”
People who believe they’re ill with the virus should contact their provider before going to a doctor’s office or an emergency room.
“I worry about ER utilization,” Ford said. “Are people going to be running to the emergency room in a panic?”
Telemedicine, where a patient consults with a doctor through a phone, also could be a valuable tool in an outbreak of a contagious disease to avoid transmission to other people in a waiting room or a doctor’s office.
“Our telemedicine and video platforms have been in place for some time and, particularly in cases such as these, provide a great resource for patients,” said Dr. Neil Gokal, a family physician with Southwest Medical Associates.
Gokal said the coronavirus also could create a new use for an old practice — the house call — by a doctor equipped with diagnostic tools found in an urgent care center.
Viral anxiety
Dr. Evelyn Montalvo Stanton, chair of pediatrics at the UNLV School of Medicine, said she’s hearing from a lot of parents concerned about COVID-19.
“The key thing is really educating parents about the coronavirus,” she said. “What are the signs and symptoms they need to look out for,” such as a cough and a fever.
“The confusing part is we’ve had such a horrible flu season this year, and the symptoms are somewhat similar,” she noted. However, to identify risk factors, practitioners have been trained to ask patients about their travel history, such as trips to China, where the majority of cases are located.
Just as with other contagious diseases, the key things that people can do to avoid getting sick involve routine practices: washing hands frequently, avoiding touching their face and disinfecting frequently touched household surfaces such as doorknobs.
Ford noted that about 80 percent of COVID-19 cases worldwide have been fairly mild, and that deaths have often been in cases complicated by other factors, such as the flu or bacterial pneumonia.
To prevent being double-teamed by the new and old diseases, Ford said, people should take the advice medical experts have been giving them for months.
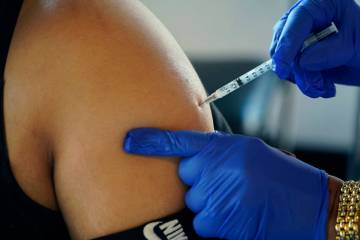
“It’s not too late to get a flu shot,” she said.
Contact Mary Hynes at mhynes@reviewjournal.com or 702-383-0336. Follow @MaryHynes1 on Twitter.
Related story
Trump names Pence to lead US response
A run on supplies
The manager of a standalone CVS store near the Las Vegas Medical District has started to enforce a one-box-per-customer policy on face masks after running out of stock on Wednesday.
The manager, who asked not to be identified, fears people are buying them in bulk and reselling them.
"One day, I (received a shipment) and got 24 boxes in and put them on the shelf and five minutes later, one lady bought all of them," the store manager said. "Someone right behind her came in looking for them and he said, 'Hey, can I buy one of those?' and she said, 'No, I'm buying them.'"
She said she has heard that buying out a store's entire stock is a problem at other CVS stores. She said she receives a shipment of inventory every two weeks.
The manager said she has never seen any instances of a customer buying the entire inventory of a product at the store until all boxes of masks were bought.
Richard N. Velotta/Las Vegas Review-Journal